Stepwise asynchronous telehealth assessment of patients with suspected axial spondyloarthritis: results from a pilot study
- PMID: 37316631
- PMCID: PMC10766678
- DOI: 10.1007/s00296-023-05360-z
Stepwise asynchronous telehealth assessment of patients with suspected axial spondyloarthritis: results from a pilot study
Abstract
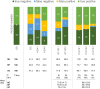
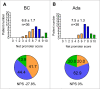
Patients with axial spondyloarthritis (axSpA) suffer from one of the longest diagnostic delays among all rheumatic diseases. Telemedicine (TM) may reduce this diagnostic delay by providing easy access to care. Diagnostic rheumatology telehealth studies are scarce and largely limited to traditional synchronous approaches such as resource-intensive video and telephone consultations. The aim of this study was to investigate a stepwise asynchronous telemedicine-based diagnostic approach in patients with suspected axSpA. Patients with suspected axSpA completed a fully automated digital symptom assessment using two symptom checkers (SC) (bechterew-check and Ada). Secondly, a hybrid stepwise asynchronous TM approach was investigated. Three physicians and two medical students were given sequential access to SC symptom reports, laboratory and imaging results. After each step, participants had to state if axSpA was present or not (yes/no) and had to rate their perceived decision confidence. Results were compared to the final diagnosis of the treating rheumatologist. 17 (47.2%) of 36 included patients were diagnosed with axSpA. Diagnostic accuracy of bechterew-check, Ada, TM students and TM physicians was 47.2%, 58.3%, 76.4% and 88.9% respectively. Access to imaging results significantly increased sensitivity of TM-physicians (p < 0.05). Mean diagnostic confidence of false axSpA classification was not significantly lower compared to correct axSpA classification for both students and physicians. This study underpins the potential of asynchronous physician-based telemedicine for patients with suspected axSpA. Similarly, the results highlight the need for sufficient information, especially imaging results to ensure a correct diagnosis. Further studies are needed to investigate other rheumatic diseases and telediagnostic approaches.
Keywords: Diagnosis; Health service research; Spondyloarthritis; Symptom checker; Telehealth; Telemedicine.
© 2023. The Author(s).
Figures
References
-
- Bohn R, Cooney M, Deodhar A, Curtis JR, Golembesky A. Incidence and prevalence of axial spondyloarthritis: methodologic challenges and gaps in the literature. Clin Exp Rheumatol. 2018;36(2):263–274. - PubMed
-
- Poddubnyy D, Sieper J, Akar S, Munoz-Fernandez S, Haibel H, Hojnik M, Ganz F, Inman RD. Characteristics of patients with axial spondyloarthritis by geographic regions: PROOF multicountry observational study baseline results. Rheumatology. 2022;61(8):3299–3308. doi: 10.1093/rheumatology/keab901. - DOI - PMC - PubMed
-
- Garrido-Cumbrera M, Navarro-Compan V, Bundy C, Mahapatra R, Makri S, Correa-Fernandez J, Christen L, Delgado-Dominguez CJ, Poddubnyy D, Group EW Identifying parameters associated with delayed diagnosis in axial spondyloarthritis: data from the European map of axial spondyloarthritis. Rheumatology. 2022;61(2):705–712. doi: 10.1093/rheumatology/keab369. - DOI - PMC - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials

