Effect of bone cement-reinforced pedicle screws combined with fusion repositioning therapy on lumbar spine function and postoperative complications in patients with severe lumbar spondylolisthesis
- PMID: 37323938
- PMCID: PMC10265474
- DOI: 10.1016/j.conctc.2023.101156
Effect of bone cement-reinforced pedicle screws combined with fusion repositioning therapy on lumbar spine function and postoperative complications in patients with severe lumbar spondylolisthesis
Abstract
Objective: To retrospectively study the efficacy of bone cement-enhanced pedicle screws combined with interbody fusion reduction in the treatment of severe lumbar spondylolisthesis, its effect on lumbar function and complications.
Methods: From January 2019 to June 2021, 82 cases of severe lumbar spondylolisthesis in our hospital were analyzed. According to the different treatment plans, the patients were divided into two groups: A and B, in which group A patients were treated with pedicle screws combined with fusion and reduction, and group B patients were treated with bone cement reinforced pedicle screws combined with fusion and reduction. Perioperative indexes, pain severity (VAS), Oswestry dysfunction index (ODI), and low back and leg pain score of Japan Orthopedic Association (JOA), spondylolisthesis reduction, intervertebral space height, intervertebral foramen height, complications, and screw loosening were compared between the two groups.
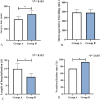
Results: There was no significant difference in the amount of intraoperative bleeding between group A and group B (P > 0.05). The operation time of group B was longer than that of group A, and the hospitalization time was shorter than that of group A. The vertebral fusion rate of group B was higher than that of group A (P < 0.05). The VAS, ODI and JOA scores at the last follow-up in both groups were lower than those before surgery, and group B was lower than group A (P < 0.05). Compared with the preoperative period, the postoperative slippage degree grading improved in both groups, while the improvement rate in group B was higher than that in group A (P < 0.05). At the last follow-up, the scores of intervertebral foramen height and intervertebral space height in both groups were higher than those before operation, and those in group B were higher than those in group A (P < 0.05). There was no difference in the incidence of complications and screw loosening between the two groups (P > 0.05).
Conclusion: Compared with conventional screw treatment, bone cement-reinforced pedicle screws combined with fusion repositioning can further improve the repositioning rate of slipped vertebrae in the treatment of severe LSL, while achieving a better intervertebral fusion rate. Therefore, the treatment of severe LSL with bone cement reinforced pedicle fusion and reduction is a safe and effective method.
Keywords: Cement-reinforced pedicle screw; Complications; Fusion repositioning; Lumbar spine function; Severe lumbar spondylolisthesis.
© 2023 Published by Elsevier Inc.
Conflict of interest statement
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Figures


Similar articles
-
[Two different fixation methods combined with lumbar interbody fusion for the treatment of two-level lumbar vertebra diseases: a clinical comparison study].Zhongguo Gu Shang. 2015 Oct;28(10):903-9. Zhongguo Gu Shang. 2015. PMID: 26727781 Chinese.
-
[Channel-assisted fixation and interbody fusion in treating recurrent lumbar disc herniation by muscle-splitting approach].Zhongguo Gu Shang. 2021 Apr 25;34(4):304-4. doi: 10.12200/j.issn.1003-0034.2021.04.003. Zhongguo Gu Shang. 2021. PMID: 33896127 Chinese.
-
[Unilateral pedicle screw fixation versus its combination with contralateral translaminar facet screw fixation for the treatment of single segmental lower lumbar vertebra diseases].Zhongguo Gu Shang. 2015 Apr;28(4):306-12. Zhongguo Gu Shang. 2015. PMID: 26072610 Chinese.
-
[Two different techniques combined with MIS-TLIF in the treatment of degenerative lumbar spondylolisthesis:a case-control study].Zhongguo Gu Shang. 2022 May 25;35(5):409-17. doi: 10.12200/j.issn.1003-0034.2022.05.002. Zhongguo Gu Shang. 2022. PMID: 35535527 Chinese.
-
Cement-augmented pedicle screw for thoracolumbar degenerative diseases with osteoporosis: a systematic review and meta-analysis.J Orthop Surg Res. 2023 Aug 28;18(1):631. doi: 10.1186/s13018-023-04077-w. J Orthop Surg Res. 2023. PMID: 37641101 Free PMC article.
References
-
- Bydon M., Alvi M.A., Goyal A. Degenerative lumbar spondylolisthesis: definition, natural history, conservative management, and surgical treatment. Neurosurg. Clin. 2019 Jul;30(3):299–304. - PubMed
-
- Ghogawala Z., Dunbar M.R., Essa I. Lumbar spondylolisthesis: modern registries and the development of artificial intelligence. J. Neurosurg. Spine. 2019 Jun 1;30(6):729–735. - PubMed
-
- Kotani Y., Koike Y., Ikeura A., Tokunaga H., Saito T. Clinical and radiologic comparison of anterior-posterior single-position lateral surgery versus MIS-TLIF for degenerative lumbar spondylolisthesis. J. Orthop. Sci. 2021 Nov;26(6):992–998. doi: 10.1016/j.jos.2020.10.013. Epub 2020 Dec 16. PMID: 33339720. - DOI - PubMed
-
- Nöst X., Pferschy-Wenzig E.M., Yu X.T., Li M., Tong X.L., Bauer R. Comprehensive metabolic profiling of modified Gegen Qinlian decoction by ultrahigh performance liquid chromatography-diodearraydetection-Q-Exactive-Orbitrap-electrosprayionization-massspectrometry/mass spectrometry and application of high-performance thin-layer chromatography. World J Tradit Chin Med. 2021;7:11–32.
LinkOut - more resources
Full Text Sources

