Efficacy and safety of botulinum toxin for treating motor dysfunction in patients with Parkinson's disease: a systematic review and meta-analysis
- PMID: 37328181
- PMCID: PMC10277107
- DOI: 10.1136/bmjopen-2021-060274
Efficacy and safety of botulinum toxin for treating motor dysfunction in patients with Parkinson's disease: a systematic review and meta-analysis
Abstract
Objective: To evaluate the efficacy and safety of botulinum toxin (BTX) for motor dysfunction in Parkinson's disease (PD).
Design: Systematic review and meta-analysis.
Data sources: Searches of PubMed, EMBASE and the Cochrane Library, from database inception to 20 October 2022.
Eligibility criteria: Studies reported in English with adult PD patients treated with BTX.
Data extraction and synthesis: Primary outcomes were United Parkinson's Disease Rate Scale Section (UPDRS) III (or its items) and Visual Analogue Scale (VAS). Secondary outcomes were UPDRS-II (or its items), Freezing of Gait Questionnaire (FOG-Q), Timed Up and Go test (TUG) and treatment-related adverse events (TRAEs). Mean difference (MD) or standardised MD (SMD) before and after treatment with 95% CIs were used for continuous variables and risk ratios (RRs) with 95% CIs was used for TRAEs.
Results: Six randomised controlled trials (RCTs) and six non-RCTs (case series) were included (ntotal=224 participants, nRCT=165). No significant difference was found in pooled results of UPDRS-III (available in four RCTs and two non-RCTs, SMD=-0.19, 95% CI -0.98 to 0.60), UPDRS-II (four RCTs and one non-RCT, SMD=-0.55, 95% CI -1.22 to 0.13), FOG-Q (one RCT and one non-RCT, SMD=0.53, 95% CI -1.93 to 2.98) or the risk of TRAEs (five RCTs, RR 0.87, 95% CI 0.37 to 2.01). Significant decreases were found in pooled VAS score (three RCTs and five non-RCTs, MD=-2.14, 95% CI -3.05 to -1.23) and TUG (MD=-2.06, 95% CI -2.91 to -1.20) after BTX treatment.
Conclusions: BTX may not be associated with motor symptoms alleviation, although it benefits pain alleviation and functional mobility improvement.
Keywords: NEUROPHYSIOLOGY; Neuropathology; Parkinson-s disease.
© Author(s) (or their employer(s)) 2023. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ.
Conflict of interest statement
Competing interests: None declared.
Figures




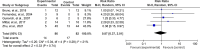
Similar articles
-
The effectiveness and safety of botulinum toxin injections for managing motor disorders of patients with Parkinson's disease: A meta-analysis of randomized controlled trials.Basic Clin Pharmacol Toxicol. 2024 Nov;135(5):655-663. doi: 10.1111/bcpt.14082. Epub 2024 Sep 19. Basic Clin Pharmacol Toxicol. 2024. PMID: 39300700
-
The effects of transcranial magnetic stimulation for freezing of gait in Parkinson's disease: a systematic review and meta-analysis of randomized controlled trials.Front Aging Neurosci. 2024 Feb 2;16:1304852. doi: 10.3389/fnagi.2024.1304852. eCollection 2024. Front Aging Neurosci. 2024. PMID: 38371401 Free PMC article.
-
Meta-analysis of randomized controlled trials of the effects of probiotics in Parkinson's disease.Food Funct. 2023 Apr 24;14(8):3406-3422. doi: 10.1039/d2fo03825k. Food Funct. 2023. PMID: 36974511 Review.
-
Botulinum toxin for chronic rhinitis: A systematic review and meta-analysis.Int Forum Allergy Rhinol. 2021 Nov;11(11):1538-1548. doi: 10.1002/alr.22813. Epub 2021 May 6. Int Forum Allergy Rhinol. 2021. PMID: 33956405
-
Botulinum toxin type B for gait freezing in Parkinson's disease.Med Sci Monit. 2004 Jul;10(7):CR282-4. Epub 2004 Jun 29. Med Sci Monit. 2004. PMID: 15232500 Clinical Trial.
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
