The impact of decentralisation on health systems in fragile and post-conflict countries: a narrative synthesis of six case studies in the Indo-Pacific
- PMID: 37340483
- PMCID: PMC10280898
- DOI: 10.1186/s13031-023-00528-7
The impact of decentralisation on health systems in fragile and post-conflict countries: a narrative synthesis of six case studies in the Indo-Pacific
Abstract
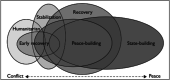
A health system has three key stakeholders, the State-at national and subnational levels-the health service providers and the citizens. In most settings and especially in peacetime, these stakeholders are typically well-defined. In contrast, during conflict and crisis as well as during ceasefire and post-conflict peacebuilding, stakeholders in the health system are often more diverse and contested. Health systems in such settings tend to be more decentralised, de facto-often in addition to de jure decentralisation. Despite much debate on the potential benefits of decentralisation, assessing its impact on health system performance remains difficult and its effect is open to dispute in the literature. This narrative synthesis aims to support efforts to assess and make sense of how decentralisation impacts health system performance in fragile and post-conflict countries-by synthesising evidence on the impact of decentralisation on health system performance from six country case studies: Papua New Guinea, the Philippines, Indonesia, Pakistan, Myanmar and Nepal. The impact of decentralisation on health system performance is optimised when combining centralisation (e.g., the benefits of central coordination in improving efficiency) with decentralisation (e.g., the benefits of local decision making in improving equity and resilience). The findings may inform efforts to think through what to centralise or decentralise, the impacts of those choices, and how the impact may change over time as countries go through and emerge from conflict-and as they go through and recover from the Covid-19 pandemic and prepare for future pandemics.
Keywords: Conflict; Fragile; Health; Health system; Peacebuilding.
© 2023. The Author(s).
Conflict of interest statement
The authors declare that they have no competing interests.
Figures
References
-
- World Health Organisation. https://www.who.int/health-topics/health-systems-governance [Internet]. [cited 2022 Mar 30].
-
- Galtung J, Fischer D. Johan Galtung pioneer of peace research. Berlin: Springer; 2013.
-
- Manor J. The political economy of democratic decentralization. Washington: World Bank; 1999.
-
- Saltman R, Bankauskaite V. Central issues in the decentralisation debate. In: Saltman RB, Bankauskaite V, Vrangbek K, editors. Decentralization in health care. New York: McGraw-Hill; 2007. pp. 9–21.
LinkOut - more resources
Full Text Sources
Research Materials