Acute non-ST segment elevation myocardial infarction as the first manifestation of Takayasu arteritis in a 16-year-old female patient: a case report and literature review
- PMID: 37340716
- PMCID: PMC10288406
- DOI: 10.1177/03000605231178599
Acute non-ST segment elevation myocardial infarction as the first manifestation of Takayasu arteritis in a 16-year-old female patient: a case report and literature review
Abstract
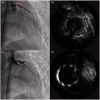
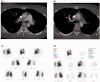
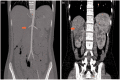
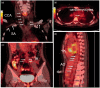
Takayasu arteritis (TA) is now recognized worldwide and is a disease that mainly affects the aorta and its main branches. TA rarely involves the small or medium-sized vessels. Certain vascular lesions, such as arterial stenosis, occlusion, and aneurysm are common with TA. However, patients with new-onset TA who present with left main trunk acute non-ST segment elevation myocardial infarction are extremely rare. We report a 16-year-old female patient with non-ST segment elevation myocardial infarction due to severe stenosis of the left main coronary artery that was caused by TA. She was eventually diagnosed with TA and underwent successful coronary artery stenting combined with glucocorticoids and folate reductase inhibitor therapy. Over the 1-year follow-up, she experienced two episodes of chest pain and was admitted to the hospital. During the second hospitalization, coronary angiography (CAG) revealed 90% stenosis of the original left main trunk (LM) stent. Following percutaneous coronary angiography (PTCA), drug-coated balloon (DCB) angioplasty was performed. Fortunately, a clear diagnosis of TA was made, and treatment was initiated with an interleukin-6 (IL-6) receptor inhibitor. Early diagnosis and therapy for TA are emphasized.
Keywords: Acute non-ST segment elevation myocardial infarction; Takayasu arteritis; chest pain; coronary artery angiography; coronary artery stenting; folate reductase inhibitor; immunosuppressive therapy; interleukin-6 receptor inhibitor.
Conflict of interest statement
The authors declare that there is no conflict of interest.
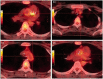
Figures



Similar articles
-
Acute myocardial infarction with left main coronary artery ostial negative remodelling as the first manifestation of Takayasu arteritis: a case report.BMC Cardiovasc Disord. 2021 Nov 22;21(1):560. doi: 10.1186/s12872-021-02376-w. BMC Cardiovasc Disord. 2021. PMID: 34809570 Free PMC article.
-
Takayasu arteritis with coronary aneurysms causing acute myocardial infarction in a young man.Tex Heart Inst J. 2011;38(2):183-6. Tex Heart Inst J. 2011. PMID: 21494533 Free PMC article.
-
Left main coronary occlusion from Takayasu arteritis in an 8-year-old child.Pediatr Cardiol. 2007 May-Jun;28(3):234-7. doi: 10.1007/s00246-006-0080-6. Epub 2007 Mar 10. Pediatr Cardiol. 2007. PMID: 17505866 Review.
-
Regressed coronary ostial stenosis in a young female with Takayasu arteritis: a case report.BMC Cardiovasc Disord. 2019 Apr 2;19(1):79. doi: 10.1186/s12872-019-1066-7. BMC Cardiovasc Disord. 2019. PMID: 30940076 Free PMC article.
-
[Acute Myocardial Infarction as a Presentation of Takayasu Arteritis in a Patient with Ulcerative Colitis: Case Report and Review of the Topic].Rev Med Chil. 2024 Jul;152(7):831-835. doi: 10.4067/s0034-98872024000700831. Rev Med Chil. 2024. PMID: 39760552 Review. Spanish.
Cited by
-
Research progress of drug eluting balloon in arterial circulatory system.Front Cardiovasc Med. 2024 Mar 20;11:1287852. doi: 10.3389/fcvm.2024.1287852. eCollection 2024. Front Cardiovasc Med. 2024. PMID: 38601040 Free PMC article. Review.
-
A Systematic Review of Anti-TNF and Anti-IL-6 Treatments for Pediatric Takayasu Arteritis: Addressing a Therapeutic Dilemma.Paediatr Drugs. 2025 Sep;27(5):563-574. doi: 10.1007/s40272-025-00706-5. Epub 2025 Jun 18. Paediatr Drugs. 2025. PMID: 40531440 Free PMC article.
References
-
- Wilson L, Chandran A, Fudge JC, et al.. Takayasu’s arteritis presenting as acute myocardial infarction: case series and review of literature. Cardiol Young 2021; 31: 1866–1869. - PubMed
-
- Cavalli G, Tomelleri A, Napoli DD, et al.. Prevalence of Takayasu arteritis in young women with acute ischemic heart disease. Int J Cardiol 2018; 252: 21–23. - PubMed
-
- Lei C, Huang Y, Yuan S, et al.. Takayasu arteritis with coronary artery involvement: differences between pediatric and adult patients. Can J Cardiol 2020; 36: 535–542. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials

