Decision-to-delivery interval and neonatal outcomes in intrapartum umbilical cord prolapse
- PMID: 37349738
- PMCID: PMC10288770
- DOI: 10.1186/s12884-023-05788-y
Decision-to-delivery interval and neonatal outcomes in intrapartum umbilical cord prolapse
Abstract
Background: Rapid delivery is important in cases of umbilical cord prolapse to prevent hypoxic injury to the fetus/neonate. However, the optimal decision-to-delivery interval remains controversial.
Objective: The aim of the study was to investigate the association between the decision-to-delivery interval in women with umbilical cord prolapse, stratified by fetal heart rate pattern at diagnosis, and neonatal outcome.
Study design: The database of a tertiary medical center was retrospectively searched for all cases of intrapartum cord prolapse between 2008 and 2021. The cohort was divided into three groups according to findings on the fetal heart tracing at diagnosis: 1) bradycardia; 2) decelerations without bradycardia; and 3) reassuring heart rate. The primary outcome measure was fetal acidosis. The correlation between cord blood indices and decision-to-delivery interval was analyzed using Spearman's rank correlation coefficient.
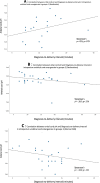
Results: Of the total 103,917 deliveries performed during the study period, 130 (0.13%) were complicated by intrapartum umbilical cord prolapse. Division by fetal heart tracing yielded 22 women (16.92%) in group 1, 41 (31.53%) in group 2, and 67 (51.53%) in group 3. The median decision-to-delivery interval was 11.0 min (IQR 9.0-15.0); the interval was more than 20 min in 4 cases. The median cord arterial blood pH was 7.28 (IQR 7.24-7.32); pH was less than 7.2 in 4 neonates. There was no correlation of cord arterial pH with decision-to-delivery interval (Spearman's Ρ = - 0.113; Ρ = 0.368) or with fetal heart rate pattern (Spearman's Ρ = .425; Ρ = .079, Ρ = - .205; Ρ = .336, Ρ = - .324; Ρ = .122 for groups 1-3, respectively).
Conclusion: Intrapartum umbilical cord prolapse is a relatively rare obstetric emergency with an overall favorable neonatal outcome if managed in a timely manner, regardless of the immediately preceding fetal heart rate. In a clinical setting which includes a high obstetric volume and a rapid, protocol-based, response, there is apparently no significant correlation between decision-to-delivery interval and cord arterial cord pH.
Keywords: Cord arterial blood pH; Cord prolapse; Decision-to-delivery interval.
© 2023. The Author(s).
Conflict of interest statement
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
The authors have no relevant financial or non-financial interests to disclose.
Figures

Similar articles
-
Bradycardia-to-delivery interval and fetal outcomes in umbilical cord prolapse.Acta Obstet Gynecol Scand. 2021 Jan;100(1):170-177. doi: 10.1111/aogs.13985. Epub 2020 Sep 14. Acta Obstet Gynecol Scand. 2021. PMID: 32862427
-
Umbilical cord prolapse: revisiting its definition and management.Am J Obstet Gynecol. 2021 Oct;225(4):357-366. doi: 10.1016/j.ajog.2021.06.077. Epub 2021 Jun 26. Am J Obstet Gynecol. 2021. PMID: 34181893 Review.
-
Umbilical cord prolapse during delivery - risk factors and pregnancy outcome: a single center experience.J Matern Fetal Neonatal Med. 2014 Jan;27(1):14-7. doi: 10.3109/14767058.2013.799651. Epub 2013 May 30. J Matern Fetal Neonatal Med. 2014. PMID: 23617536
-
Urgent cesarean delivery for fetal bradycardia.Obstet Gynecol. 2009 Nov;114(5):1023-1028. doi: 10.1097/AOG.0b013e3181bc6e15. Obstet Gynecol. 2009. PMID: 20168102
-
Umbilical cord prolapse.Obstet Gynecol Clin North Am. 2013 Mar;40(1):1-14. doi: 10.1016/j.ogc.2012.11.002. Obstet Gynecol Clin North Am. 2013. PMID: 23466132 Review.
Cited by
-
Incidence and predictors of mortality among neonates admitted with birth asphyxia to neonatal intensive care units in Ethiopia: a systematic review and meta-analysis.BMC Pediatr. 2025 Feb 26;25(1):140. doi: 10.1186/s12887-025-05481-3. BMC Pediatr. 2025. PMID: 40001015 Free PMC article.
References
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

