Diagnostic Value and Prognosis Significance of Cerebrospinal Fluid Examination by Flow Cytometry in Pediatric Acute Lymphoblastic Leukemia
- PMID: 37350078
- PMCID: PMC10302597
- DOI: 10.1177/15330338231181025
Diagnostic Value and Prognosis Significance of Cerebrospinal Fluid Examination by Flow Cytometry in Pediatric Acute Lymphoblastic Leukemia
Abstract
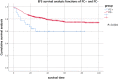
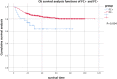
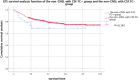
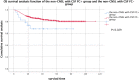
Purpose: To explore the diagnostic value and the prognostic significance of cerebrospinal fluid (CSF) examination by flow cytometry (FC) in children with central nervous system leukemia (CNSL). Method: This is a retrospective observational study. We select 986 pediatric patients with newly diagnosed acute lymphoblastic leukemia from January 2012 to December 2018 as the research objects and analyze the sensitivity and specificity of different methods for diagnosing CNSL. The recurrence rate and survival rate of CNSL in different groups were compared. Results: Among the 986 cases, 31 cases (positive rate of 3.14%) were positive by FC, and the cytospin-based cytomorphology (CC) test was positive in 6 cases (positive rate of 0.61%). CC combined with FC might improve the diagnostic sensitivity (from 30% to 65%, 𝑥2 value was 5.143, P = .016). The 2-year event-free survival (EFS) of 31 FC + children was 59.5% ± 9.2%, and that of 955 FC - children was 74.1% ± 1.8% (P = .004). The 2-year overall survival (OS) of the 2 groups were 63.6% ± 9.7% and 80.2% ± 1.5%, respectively (P = .004). In order to exclude the influence of CNSL, we divided the patients into 3 groups: CNSL group and non-CNSL group with CSF FC + , FC - group. There was no significant difference in EFS between FC - group and non-CNSL group with FC + (2-year EFS were 74.1% ± 1.8% and 68.7% ± 9.8%, respectively, P = .142), and there was a significant difference in OS (2-year OS were 80.2% ± 1.5% and 67.5% ± 10.3%, respectively, P = .029). Conclusion: The test of FC combined with CC may improve the diagnostic sensitivity of CNSL. The EFS and OS of children with FC + are worse than those of children with FC -. However, for those patients with non-CNSL, but only FC + at the initial diagnosis, the EFS is not significantly affected by strengthening systemic chemotherapy and increasing the number of intrathecal injections.
Keywords: acute lymphoblastic leukemia; central nervous system leukemia; cerebrospinal fluid; children; flow cytometry.
Conflict of interest statement
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Figures
Similar articles
-
Diagnostic significance of cerebrospinal fluid flow cytometry in Chinese children with B lineage acute lymphoblastic leukemia.BMC Pediatr. 2024 Mar 22;24(1):204. doi: 10.1186/s12887-024-04684-4. BMC Pediatr. 2024. PMID: 38519960 Free PMC article.
-
[Clinical diagnostic significance of cerebrospinal fluid detection with flow cytometry in children acute lymphoblastic leukemia accompanied by central nervous system leukemia].Zhongguo Shi Yan Xue Ye Xue Za Zhi. 2012 Feb;20(1):38-42. Zhongguo Shi Yan Xue Ye Xue Za Zhi. 2012. PMID: 22391161 Chinese.
-
Characteristics of Central Nervous System (CNS) Involvement in Children With Non-Hodgkin's Lymphoma (NHL) and the Diagnostic Value of CSF Flow Cytometry in CNS Positive Disease.Technol Cancer Res Treat. 2021 Jan-Dec;20:15330338211016372. doi: 10.1177/15330338211016372. Technol Cancer Res Treat. 2021. PMID: 34060372 Free PMC article.
-
Obesity as the initial manifestation of central nervous system relapse of acute lymphoblastic leukemia: case report and literature review.J Cancer Res Ther. 2012 Jan-Mar;8(1):151-3. doi: 10.4103/0973-1482.95200. J Cancer Res Ther. 2012. PMID: 22531539 Review.
-
New attempts for central nervous infiltration of pediatric acute lymphoblastic leukemia.Cancer Metastasis Rev. 2019 Dec;38(4):657-671. doi: 10.1007/s10555-019-09827-z. Cancer Metastasis Rev. 2019. PMID: 31820149 Review.
References
-
- Schultz KR, Pullen DJ, Sather HN, et al.Risk- and response-based classification of childhood B-precursor acute lymphoblastic leukemia: a combined analysis of prognostic markers from the pediatric oncology group (POG) and children’s cancer group (CCG). Blood. 2007;109(3):926‐935. doi: 10.1182/blood-2006-01-024729. - DOI - PMC - PubMed
-
- Winick N, Devidas M, Chen S, et al.Impact of initial CSF findings on outcome among patients with national cancer institute standard- and high-risk B-cell acute lymphoblastic leukemia: a report from the children’s oncology group. J Clin Oncol. 2017;35(22):2527‐2534. doi: 10.1200/JCO.2016.71.4774. - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources

