Collagen Hydrolysate Effects on Photodynamic Efficiency of Gallium (III) Phthalocyanine on Pigmented Melanoma Cells
- PMID: 37367145
- PMCID: PMC10297862
- DOI: 10.3390/gels9060475
Collagen Hydrolysate Effects on Photodynamic Efficiency of Gallium (III) Phthalocyanine on Pigmented Melanoma Cells
Abstract
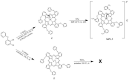
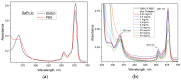
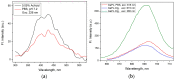
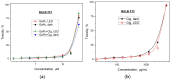
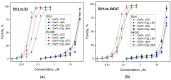
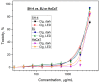
The conjugation of photosensitizer with collagen seems to be a very promising approach for innovative topical photodynamic therapy (PDT). The study aims to evaluate the effects of bovine collagen hydrolysate (Clg) on the properties of gallium (III) phthalocyanine (GaPc) on pigmented melanoma. The interaction of GaPc with Clg to form a conjugate (GaPc-Clg) showed a reduction of the intensive absorption Q-band (681 nm) with a blue shift of the maximum (678 nm) and a loss of shape of the UV-band (354 nm). The fluorescence of GaPc, with a strong emission peak at 694 nm was blue shifted due to the conjugation which lower intensity owing to reduce quantum yield (0.012 vs. 0.23, GaPc). The photo- and dark cytotoxicity of GaPc, Glg and GaPc-Clg on pigmented melanoma cells (SH-4) and two normal cell lines (BJ and HaCaT) showed a slight decrease of cytotoxicity for a conjugate, with low selectivity index (0.71 vs. 1.49 for GaPc). The present study suggests that the ability of collagen hydrolysate to form gels minimizes the high dark toxicity of GaPc. Collagen used for conjugation of a photosensitizer might be an essential step in advanced topical PDT.
Keywords: bovine collagen hydrolysate and gels; gallium phthalocyanine; mouse embryonal fibroblasts; normal keratocytes and fibroblasts; photodynamic therapy; pigmented melanoma.
Conflict of interest statement
The authors declare no conflict of interest. The funder had no role in the design of the study; in the collection, analyses, or interpretation of data; in the writing of the manuscript, or in the decision to publish the results.
Figures
References
-
- Sharma D., Singh S., Kumar P., Jain G.K., Aggarwal G., Almalki W.H., Kesharwani P. 2—Mechanisms of Photodynamic Therapy. In: Kesharwani P., editor. Nanomaterials for Photodynamic Therapy. Woodhead Publishing; Sawston, UK: 2023. pp. 41–54. (Woodhead Publishing Series in Biomaterials). - DOI
Grants and funding
LinkOut - more resources
Full Text Sources

