Single-center initial experience with inner-branch complex EVAR in 44 patients
- PMID: 37396572
- PMCID: PMC10309562
- DOI: 10.3389/fcvm.2023.1188501
Single-center initial experience with inner-branch complex EVAR in 44 patients
Abstract
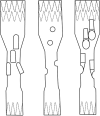
Purpose: The use of inner-branch aortic stent grafts in the treatment of complex aortic pathologies aims at broad applicability and stable bridging stent sealing compared to other endovascular technologies. The objective of this study was to evaluate the early outcomes with a single manufacturer custom-made and off-the-shelf inner-branched endograft in a mixed patient cohort.
Methods: This retrospective, monocentric study between 2019 and 2022 included 44 patients treated with inner-branched aortic stent grafts (iBEVAR) as custom-made device (CMD) or off-the-shelf device (E-nside) with at least four inner branches. The primary endpoints were technical and clinical success.
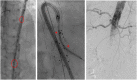
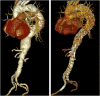
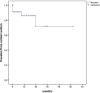
Results: Overall, 77% (n = 34) and 23% (n = 10) of the patients (mean age 77 ± 6.5 years, n = 36 male) were treated with a custom-made iBEVAR with at least four inner branches and an off-the-shelf graft, respectively. Treatment indications were thoracoabdominal pathologies in 52.2% (n = 23), complex abdominal aneurysms in 25% (n = 11), and type Ia endoleaks in 22.7% (n = 10). Preoperative spinal catheter placement was performed in 27% (n = 12) of patients. Implantation was entirely percutaneous in 75% (n = 33). Technical success was 100%. Target vessel success manifested at 99% (178/180). There was no in-hospital mortality. Permanent paraplegia developed in 6.8% (n = 3) of patients. The mean follow-up was 12 months (range 0-52 months). Three late deaths (6.8%) occurred, one related to an aortic graft infection. Kaplan-Meier estimated 1-year survival manifested at 95% and branch patency at 98% (177/180). Re-intervention was necessary for a total of six patients (13.6%).
Conclusions: Inner-branch aortic stent grafts provide a feasible option for the treatment of complex aortic pathologies, both elective (custom-made) and urgent (off-the-shelf). The technical success rate is high with acceptable short-term outcomes and moderate re-intervention rates comparable to existing platforms. Further follow-up will evaluate long-term outcomes.
Keywords: aortic stent graft; complex endovascular aortic repair; inner branches; off-the-shelf; thoracoabdominal aneurysm repair.
© 2023 Kapalla, Busch, Lutz, Nebelung, Wolk and Reeps.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures

References
-
- Gallitto E, Faggioli G, Melissano G, Fargion A, Isernia G, Lenti M, et al. Preoperative and postoperative predictors of clinical outcome of fenestrated and branched endovascular repair for complex abdominal and thoracoabdominal aortic aneurysms in an Italian multicenter registry. J Vasc Surg. (2021) 74(6):1795–806.e6. 10.1016/j.jvs.2021.04.072 - DOI - PubMed
LinkOut - more resources
Full Text Sources

