The eliminate hepatitis C (EC) experience study: baseline characteristics of a cohort of people who inject drugs in Melbourne, Australia
- PMID: 37400235
- PMCID: PMC10335404
- DOI: 10.1136/bmjopen-2023-071665
The eliminate hepatitis C (EC) experience study: baseline characteristics of a cohort of people who inject drugs in Melbourne, Australia
Abstract
Objectives: Direct-acting antivirals provide an opportunity to eliminate hepatitis C virus (HCV) as a public health threat in Australia, yet barriers to care remain. In this study, we use baseline data from a longitudinal cohort of people who inject drugs to understand differences in participant characteristics and explore experiences of stigma, health service utilisation and health literacy between three care cascade groups.
Design: Cross-sectional.
Setting: Community and private primary healthcare services in Melbourne, Australia.
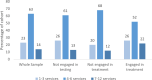
Participants: Participants completed baseline surveys between 19 September 2018 and 15 December 2020. We recruited 288 participants; the median age was 42 years (IQR: 37-49 years) and 198 (69%) were male. At baseline, 103 (36%) self-reported being 'not engaged in testing', 127 (44%) had HCV RNA positivity but were 'not engaged in treatment' and 58 (20%) were 'engaged in HCV treatment'.
Outcome measures: Descriptive statistics were used to present the baseline demographics, health service utilisation and experiences of stigma data. We explored differences in these scales between participant demographics using χ2 test or fisher's exact tests, and differences between health literacy scores using one-way analysis of variance tests.
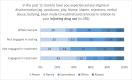
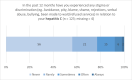
Results: A majority were in regular contact with multiple health services, and most had previously been identified as at-risk of HCV. In the 12 months preceding baseline, 70% reported any experiences of stigma related to injecting drug use. Assessment of health literacy data identified gaps for those 'not engaged in testing' and 'not engaged in treatment' across two relevant domains: 'ability to appraise health information' and 'ability to actively engage with healthcare providers'.
Conclusion: In eliminate hepatitis C experience, lower HCV testing and treatment may be explained by experiences of stigmatisation or gaps in health literacy. Enhanced interventions targeting people who inject drugs to promote HCV care are needed.
Keywords: Health Services Accessibility; Health policy; Public health.
© Author(s) (or their employer(s)) 2023. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ.
Conflict of interest statement
Competing interests: JD, MH, MAS and AP receive investigator-initiated research funding support from Gilead Sciences, Abbvie and Bristol-Myers Squibb and Merck. JD and his institution have received consultancies from Gilead, AbbVie and Merck. AP and their institution have received consultancies from Gilead. PH receives investigator-initiated research funding support from Gilead Sciences and Abbvie. PD has received an investigator-driven grant from Gilead Sciences for unrelated work on hepatitis C and an untied educational grant from Reckitt Benckiser for unrelated work on the introduction of buprenorphine-naloxone into Australia. He has served as an unpaid member on an Advisory Board for an intranasal naloxone product.
Figures
References
-
- World Health Organization . Global health sector strategy on viral hepatitis 2016-2021. 2016.
-
- Burnet Institute and Kirby Institute . Australia’s progress towards hepatitis C elimination: annual report 2022. 2022.
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
