Dissimilar survival and clinicopathological characteristics of mucinous adenocarcinoma located in pancreatic head and body/tail
- PMID: 37405087
- PMCID: PMC10315121
- DOI: 10.4240/wjgs.v15.i6.1178
Dissimilar survival and clinicopathological characteristics of mucinous adenocarcinoma located in pancreatic head and body/tail
Abstract
Background: Growing evidence shows that pancreatic tumors in different anatomical locations have different characteristics, which have a significant impact on prognosis. However, no study has reported the differences between pancreatic mucinous adenocarcinoma (PMAC) in the head vs the body/tail of the pancreas.
Aim: To investigate the differences in survival and clinicopathological characteristics between PMAC in the head and body/tail of pancreas.
Methods: A total of 2058 PMAC patients from the Surveillance, Epidemiology, and End Results database diagnosed between 1992 and 2017 were retrospectively reviewed. We divided the patients who met the inclusion criteria into pancreatic head group (PHG) and pancreatic body/tail group (PBTG). The relationship between two groups and risk of invasive factors was identified using logistic regression analysis. Kaplan-Meier analysis and Cox regression analysis were conducted to compare the overall survival (OS) and cancer-specific survival (CSS) of two patient groups.
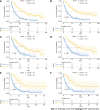
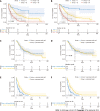
Results: In total, 271 PMAC patients were included in the study. The 1-year, 3-year, and 5-year OS rates of these patients were 51.6%, 23.5%, and 13.6%, respectively. The 1-year, 3-year, and 5-year CSS rates were 53.2%, 26.2%, and 17.4%, respectively. The median OS of PHG patients was longer than that of PBTG patients (18 vs 7.5 mo, P < 0.001). Compared to PHG patients, PBTG patients had a greater risk of metastases [odds ratio (OR) = 2.747, 95% confidence interval (CI): 1.628-4.636, P < 0.001] and higher staging (OR = 3.204, 95% CI: 1.895-5.415, P < 0.001). Survival analysis revealed that age < 65 years, male sex, low grade (G1-G2), low stage, systemic therapy, and PMAC located at the pancreatic head led to longer OS and CSS (all P < 0.05). The location of PMAC was an independent prognostic factor for CSS [hazard ratio (HR) = 0.7, 95%CI: 0.52-0.94, P = 0.017]. Further analysis demonstrated that OS and CSS of PHG were significantly better than PBTG in advanced stage (stage III-IV).
Conclusion: Compared to the pancreatic body/tail, PMAC located in the pancreatic head has better survival and favorable clinicopathological characteristics.
Keywords: Anatomical location; Pancreatic body/tail; Pancreatic head; Pancreatic mucinous adenocarcinoma; Survival.
©The Author(s) 2023. Published by Baishideng Publishing Group Inc. All rights reserved.
Conflict of interest statement
Conflict-of-interest statement: The authors have declared that no competing interest exists.
Figures





References
-
- Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, Bray F. Global Cancer Statistics 2020: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries. CA Cancer J Clin. 2021;71:209–249. - PubMed
-
- Conlon KC. Intraductal papillary mucinous tumors of the pancreas. J Clin Oncol. 2005;23:4518–4523. - PubMed
-
- Ling Q, Xu X, Zheng SS, Kalthoff H. The diversity between pancreatic head and body/tail cancers: clinical parameters and in vitro models. Hepatobiliary Pancreat Dis Int. 2013;12:480–487. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous

