Practical guidance to reduce radiation exposure in electrophysiology applying ultra low-dose protocols: a European Heart Rhythm Association review
- PMID: 37410906
- PMCID: PMC10365833
- DOI: 10.1093/europace/euad191
Practical guidance to reduce radiation exposure in electrophysiology applying ultra low-dose protocols: a European Heart Rhythm Association review
Abstract
Interventional electrophysiology offers a great variety of treatment options to patients suffering from symptomatic cardiac arrhythmia. Catheter ablation of supraventricular and ventricular tachycardia has globally evolved a cornerstone in modern arrhythmia management. Complex interventional electrophysiological procedures engaging multiple ablation tools have been developed over the past decades. Fluoroscopy enabled interventional electrophysiologist throughout the years to gain profound knowledge on intracardiac anatomy and catheter movement inside the cardiac cavities and hence develop specific ablation approaches. However, the application of X-ray technologies imposes serious health risks to patients and operators. To reduce the use of fluoroscopy during interventional electrophysiological procedures to the possibly lowest degree and to establish an optimal protection of patients and operators in cases of fluoroscopy is the main goal of modern radiation management. The present manuscript gives an overview of possible strategies of fluoroscopy reduction and specific radiation protection strategies.
Keywords: Radiation awareness; Radiation dosage reduction; Radiation protection; Ultra low-dose protocols.
© The Author(s) 2023. Published by Oxford University Press on behalf of the European Society of Cardiology.
Conflict of interest statement
Conflict of interest: P.S. is a member of the Advisory Board of Abbott, Biosense Webster, Boston Scientific, and Medtronic. V.S. has no conflicts of interest to declare. M.A. is a consultant for Biosense Webster and Boston Scientific, clinical proctor for Medtronic, and has received educational grants from Abbott. R.T. is a consultant for Biosense Webster, Abbott, and Boston Scientific, and a speaker for Medtronic. H.L. has no conflicts of interest to declare. A.B. is a consultant for Biotronik, Abbott, and Biosense Webster, clinical proctor for Biotronik and Abbott, and has received educational grants from Boston Scientific.
Figures

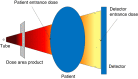
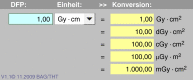
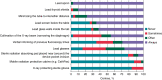
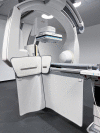
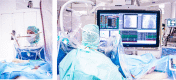

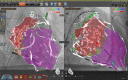
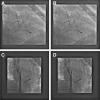
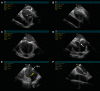
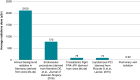
References
-
- Walters TE, Kistler PM, Morton JB, Sparks PB, Halloran K, Kalman JM. Impact of collimation on radiation exposure during interventional electrophysiology. Europace 2012;14:1670–3. - PubMed
-
- Suzuki S, Furui S, Yamakawa T, Isshiki T, Watanabe A, Iino Ret al. . Radiation exposure to patients’ skin during cardiac resynchronization therapy. Europace 2009;11:1683–8.. - PubMed
-
- Rehani MM, Vano E, Ciraj-Bielac O, Kleiman NJ. Radiation and cataract. Radiat Prot Dosimetry 2011;147:300–4. - PubMed
-
- Stewart FA, Akleyev AV, Hauer-Jensen M, Hendry JH, Kleiman NJ, Macvittie TJet al. . ICRP statement on tissue reactions and early and late effects of radiation in normal tissues and organs—threshold doses for tissue reactions in a radiation protection context. Ann ICRP 2012;41:1–322. - PubMed

