Evaluation of α-synuclein in CNS-originating extracellular vesicles for Parkinsonian disorders: A systematic review and meta-analysis
- PMID: 37416941
- PMCID: PMC10651986
- DOI: 10.1111/cns.14341
Evaluation of α-synuclein in CNS-originating extracellular vesicles for Parkinsonian disorders: A systematic review and meta-analysis
Abstract
Background & aims: Parkinsonian disorders, such as Parkinson's disease (PD), multiple system atrophy (MSA), dementia with Lewy bodies (DLB), progressive supranuclear palsy (PSP) and corticobasal syndrome (CBS), share early motor symptoms but have distinct pathophysiology. As a result, accurate premortem diagnosis is challenging for neurologists, hindering efforts for disease-modifying therapeutic discovery. Extracellular vesicles (EVs) contain cell-state-specific biomolecules and can cross the blood-brain barrier to the peripheral circulation, providing a unique central nervous system (CNS) insight. This meta-analysis evaluated blood-isolated neuronal and oligodendroglial EVs (nEVs and oEVs) α-synuclein levels in Parkinsonian disorders.
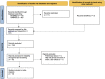
Methods: Following PRISMA guidelines, the meta-analysis included 13 studies. An inverse-variance random-effects model quantified effect size (SMD), QUADAS-2 assessed risk of bias and publication bias was evaluated. Demographic and clinical variables were collected for meta-regression.
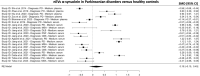
Results: The meta-analysis included 1,565 patients with PD, 206 with MSA, 21 with DLB, 172 with PSP, 152 with CBS and 967 healthy controls (HCs). Findings suggest that combined concentrations of nEVs and oEVs α-syn is higher in patients with PD compared to HCs (SMD = 0.21, p = 0.021), while nEVs α-syn is lower in patients with PSP and CBS compared to patients with PD (SMD = -1.04, p = 0.0017) or HCs (SMD = -0.41, p < 0.001). Additionally, α-syn in nEVs and/or oEVs did not significantly differ in patients with PD vs. MSA, contradicting the literature. Meta-regressions show that demographic and clinical factors were not significant predictors of nEVs or oEVs α-syn concentrations.
Conclusion: The results highlight the need for standardized procedures and independent validations in biomarker studies and the development of improved biomarkers for distinguishing Parkinsonian disorders.
Keywords: Diagnosis; L1CAM; Parkinson's disease; extracellular vesicles; α-Synuclein.
© 2023 The Authors. CNS Neuroscience & Therapeutics Published by John Wiley & Sons Ltd.
Conflict of interest statement
The authors declare no conflict of interest.
Figures






Similar articles
-
Analysis of biomarkers in speculative CNS-enriched extracellular vesicles for parkinsonian disorders: a comprehensive systematic review and diagnostic meta-analysis.J Neurol. 2024 Apr;271(4):1680-1706. doi: 10.1007/s00415-023-12093-3. Epub 2023 Dec 16. J Neurol. 2024. PMID: 38103086 Free PMC article.
-
DNA methylation patterns in the frontal lobe white matter of multiple system atrophy, Parkinson's disease, and progressive supranuclear palsy: a cross-comparative investigation.Acta Neuropathol. 2024 Jul 12;148(1):4. doi: 10.1007/s00401-024-02764-4. Acta Neuropathol. 2024. PMID: 38995454 Free PMC article.
-
Cholinesterase inhibitors for dementia with Lewy bodies, Parkinson's disease dementia and cognitive impairment in Parkinson's disease.Cochrane Database Syst Rev. 2012 Mar 14;2012(3):CD006504. doi: 10.1002/14651858.CD006504.pub2. Cochrane Database Syst Rev. 2012. PMID: 22419314 Free PMC article.
-
Tissue Factor and Its Cerebrospinal Fluid Protein Profiles in Parkinson's Disease.J Parkinsons Dis. 2024;14(7):1405-1416. doi: 10.3233/JPD-240115. J Parkinsons Dis. 2024. PMID: 39240648 Free PMC article.
-
Extracellular Vesicles for the Diagnosis of Parkinson's Disease: Systematic Review and Meta-Analysis.Mov Disord. 2023 Sep;38(9):1585-1597. doi: 10.1002/mds.29497. Epub 2023 Jul 14. Mov Disord. 2023. PMID: 37449706
Cited by
-
Biomarker bust: meta-analyses reveal unreliability of neuronal extracellular vesicles for diagnosing parkinsonian disorders.Neural Regen Res. 2025 Jan 1;20(1):201-202. doi: 10.4103/NRR.NRR-D-23-02102. Epub 2024 Apr 3. Neural Regen Res. 2025. PMID: 39657090 Free PMC article. No abstract available.
-
Synchronous monitoring of brain-heart electrophysiology using heart rate variability coupled with rapid quantitative electroencephalography in orthostatic hypotension patients with α-synucleinopathies: Rapid prediction of orthostatic hypotension and preliminary exploration of brain stimulation therapy.CNS Neurosci Ther. 2024 Feb;30(2):e14571. doi: 10.1111/cns.14571. CNS Neurosci Ther. 2024. PMID: 38421092 Free PMC article.
-
Brain white matter changes and their associations with non-motor dysfunction in orthostatic hypotension in α-synucleinopathy: A NODDI study.CNS Neurosci Ther. 2024 Apr;30(4):e14712. doi: 10.1111/cns.14712. CNS Neurosci Ther. 2024. PMID: 38615364 Free PMC article.
-
Analysis of biomarkers in speculative CNS-enriched extracellular vesicles for parkinsonian disorders: a comprehensive systematic review and diagnostic meta-analysis.J Neurol. 2024 Apr;271(4):1680-1706. doi: 10.1007/s00415-023-12093-3. Epub 2023 Dec 16. J Neurol. 2024. PMID: 38103086 Free PMC article.
-
Rethinking the reliability and accuracy of biomarkers in CNS-originating EVs for Parkinson's disease and multiple system atrophy.Front Neurol. 2023 Sep 5;14:1192115. doi: 10.3389/fneur.2023.1192115. eCollection 2023. Front Neurol. 2023. PMID: 37731853 Free PMC article. No abstract available.
References
-
- Postuma RB, Berg D, Stern M, et al. MDS clinical diagnostic criteria for Parkinson's disease. Mov Disord. 2015;30(12):1591‐1601. - PubMed
-
- Poewe W, Seppi K, Tanner CM, et al. Parkinson disease. Nat Rev Dis Primers. 2017;3:17013. - PubMed
-
- Surguchov A. Biomarkers in Parkinson's disease. In: Peplow PV, Martinez B, Gennarelli AT, eds. Neurodegenerative Diseases Biomarkers: Towards Translating Research to Clinical Practice. Humana; 2022.
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

