Sodium-Glucose Cotransporter-2 Inhibitors After Acute Myocardial Infarction in Patients With Type 2 Diabetes: A Population-Based Investigation
- PMID: 37421263
- PMCID: PMC10382092
- DOI: 10.1161/JAHA.122.027824
Sodium-Glucose Cotransporter-2 Inhibitors After Acute Myocardial Infarction in Patients With Type 2 Diabetes: A Population-Based Investigation
Abstract
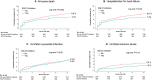
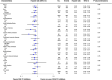
Background Whether the early use of sodium-glucose cotransporter-2 (SGLT2) inhibitors have cardioprotective effects following acute myocardial infarction is unknown. Thus, we aimed to evaluate the association between the early initiation of SGLT2 inhibitors and cardiac event rates in patients with diabetes with acute myocardial infarction undergoing percutaneous coronary intervention. Methods and Results Based on the National Health Insurance claims data in South Korea, patients who received percutaneous coronary intervention for acute myocardial infarction between 2014 and 2018 were analyzed. Patients given SGLT2 inhibitors or other glucose-lowering drugs were matched based on a propensity score. The primary end point was a composite of all-cause mortality and hospitalizations for heart failure. Major adverse cardiac events (a composite of all-cause death, nonfatal myocardial infarction, and ischemic stroke) were compared as the secondary end point. After 1:2 propensity score matching, the SGLT2 inhibitors group (938 patients) and the no use of SGLT2 inhibitors group (1876 patients) were compared. During a median follow-up of 2.1 years, the early use of SGLT2 inhibitors was associated with lower risks of both the primary end point (9.8% versus 13.9%; adjusted hazard ratio [HR], 0.68 [95% CI, 0.54-0.87]; P=0.002) and secondary end point (9.1% versus 11.6%; adjusted HR, 0.77 [95% CI, 0.60-0.99]; P=0.04). All-cause mortality and hospitalizations for heart failure were also significantly lower in early users of SGLT2 inhibitors. Conclusions The early use of SGLT2 inhibitors in patients with diabetes treated with percutaneous coronary intervention for acute myocardial infarction was associated with a significantly lower risk of cardiovascular events, including all-cause mortality, hospitalizations for heart failure, and major adverse cardiac events.
Keywords: acute myocardial infarction; diabetes; heart failure; mortality; sodium‐glucose cotransporter 2 inhibitors.
Figures


Comment in
-
So Much to Say on the Best of What's Around Regarding Sodium-Glucose Cotransporter-2 Inhibitors in Acute Myocardial Infarction.J Am Heart Assoc. 2023 Jul 18;12(14):e030495. doi: 10.1161/JAHA.123.030495. Epub 2023 Jul 8. J Am Heart Assoc. 2023. PMID: 37421265 Free PMC article. No abstract available.
References
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

