Does Malignancy Status Effect Outcomes in Patients With Large Vessel Occlusion Stroke and Cancer Who Underwent Endovascular Thrombectomy?
- PMID: 37421277
- PMCID: PMC10382110
- DOI: 10.1161/JAHA.123.029635
Does Malignancy Status Effect Outcomes in Patients With Large Vessel Occlusion Stroke and Cancer Who Underwent Endovascular Thrombectomy?
Abstract
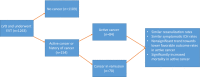
Background Cancer is associated with an increased risk of acute ischemic stroke, including large vessel occlusions. Whether cancer status affects outcomes in patients with large vessel occlusions that undergo endovascular thrombectomy remains unknown. Methods and Results All consecutive patients undergoing endovascular thrombectomy for large vessel occlusions were recruited into a prospective ongoing multicenter database, and the data were retrospectively analyzed. Patients with active cancer were compared with patients with cancer in remission. Association of cancer status with 90-day functional outcome and mortality were calculated in multivariable analyses. We identified 154 patients with cancer and large vessel occlusions that underwent endovascular thrombectomy (mean age, 74±11; 43% men; median National Institutes of Health Stroke Scale 15). Of the included patients, 70 (46%) had a remote history of cancer or cancer in remission, and 84 (54%) had active disease. Outcome data at 90 days poststroke were available for 138 patients (90%) and was classified as favorable in 53 (38%). Patients with active cancer were younger and more often smoked but did not significantly differ from those without malignancy in other risk factors, stroke severity, stroke subtype, or procedural variables. Favorable outcome rates among patients with active cancer did not significantly differ compared with those seen in patients without active cancer, but mortality rates were significantly higher among patients with active cancer on univariate and multivariable analyses. Conclusions Our study suggests that endovascular thrombectomy is safe and efficacious in patients with history of malignancy as well as in those with active cancer at the time of stroke onset, although mortality rates are higher among patients with active cancer.
Keywords: cancer; stroke; thrombectomy.
Figures
Similar articles
-
Effects of tumor type on outcomes in patients with large vessel occlusion stroke and cancer.J Stroke Cerebrovasc Dis. 2023 Sep;32(9):107288. doi: 10.1016/j.jstrokecerebrovasdis.2023.107288. Epub 2023 Aug 3. J Stroke Cerebrovasc Dis. 2023. PMID: 37542761
-
Effect of Intravenous Tirofiban vs Placebo Before Endovascular Thrombectomy on Functional Outcomes in Large Vessel Occlusion Stroke: The RESCUE BT Randomized Clinical Trial.JAMA. 2022 Aug 9;328(6):543-553. doi: 10.1001/jama.2022.12584. JAMA. 2022. PMID: 35943471 Free PMC article. Clinical Trial.
-
Endovascular Therapy is Effective for Large Vessel Occlusion Despite Concurrent Cancer.J Stroke Cerebrovasc Dis. 2022 Jun;31(6):106439. doi: 10.1016/j.jstrokecerebrovasdis.2022.106439. Epub 2022 Mar 18. J Stroke Cerebrovasc Dis. 2022. PMID: 35313233
-
Outcomes and Complications of Endovascular Mechanical Thrombectomy in the Treatment of Acute Posterior Circulation Occlusions: A Systematic Review.World Neurosurg. 2021 Jan;145:35-44. doi: 10.1016/j.wneu.2020.08.221. Epub 2020 Sep 3. World Neurosurg. 2021. PMID: 32891832
-
Predictors of first pass effect and effect on outcomes in mechanical thrombectomy for basilar artery occlusion.J Clin Neurosci. 2022 Aug;102:49-53. doi: 10.1016/j.jocn.2022.06.005. Epub 2022 Jun 17. J Clin Neurosci. 2022. PMID: 35724438 Review.
Cited by
-
Systemic Comorbidities as Modifiers of Outcome After Endovascular Thrombectomy for Acute Ischemic Stroke.Curr Neurol Neurosci Rep. 2025 May 30;25(1):38. doi: 10.1007/s11910-025-01427-5. Curr Neurol Neurosci Rep. 2025. PMID: 40442497 Review.
-
Long-term outcomes of mechanical thrombectomy in acute ischaemic stroke patients with concomitant malignancy.Postepy Kardiol Interwencyjnej. 2024 Mar;20(1):95-102. doi: 10.5114/aic.2024.137433. Epub 2024 Mar 25. Postepy Kardiol Interwencyjnej. 2024. PMID: 38616929 Free PMC article.
-
Endovascular treatment in ischemic stroke with active cancer: retrospective analysis of university stroke center data.Neurol Res Pract. 2025 May 19;7(1):34. doi: 10.1186/s42466-025-00392-1. Neurol Res Pract. 2025. PMID: 40383812 Free PMC article.
-
Acute ischaemic stroke in active cancer versus non-cancer patients: stroke characteristics, mechanisms and clinical outcomes.Eur J Neurol. 2024 Apr;31(4):e16200. doi: 10.1111/ene.16200. Epub 2024 Jan 18. Eur J Neurol. 2024. PMID: 38235924 Free PMC article.
-
Outcomes of patients with in-hospital stroke with and without active cancer.J Thromb Thrombolysis. 2025 May 27. doi: 10.1007/s11239-025-03117-y. Online ahead of print. J Thromb Thrombolysis. 2025. PMID: 40425988
References
-
- Bhave M, Akhter N, Rosen ST. Cardiovascular toxicity of biologic agents for cancer therapy. Oncology (Williston Park). 2014;28:482–490. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical