Association of GSDMD with microvascular-ischemia reperfusion injury after ST-elevation myocardial infarction
- PMID: 37424923
- PMCID: PMC10325858
- DOI: 10.3389/fcvm.2023.1138352
Association of GSDMD with microvascular-ischemia reperfusion injury after ST-elevation myocardial infarction
Abstract
Objectives: Little is known about the clinical prognosis of gasdermin D (GSDMD) in patients with ST-elevation myocardial infarction (STEMI). The purpose of this study was to investigate the association of GSDMD with microvascular injury, infarction size (IS), left ventricular ejection fraction (LVEF), and major adverse cardiac events (MACEs), in STEMI patients with primary percutaneous coronary intervention (pPCI).
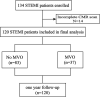
Methods: We retrospectively analyzed 120 prospectively enrolled STEMI patients (median age 53 years, 80% men) treated with pPCI between 2020 and 2021 who underwent serum GSDMD assessment and cardiac magnetic resonance (CMR) within 48 h post-reperfusion; CMR was also performed at one year follow-up.
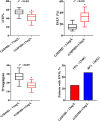
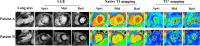
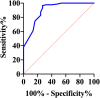
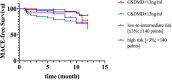
Results: Microvascular obstruction was observed in 37 patients (31%). GSDMD concentrations ≧ median (13 ng/L) in patients were associated with a higher risk of microvascular obstruction and IMH (46% vs. 19%, P = 0.003; 31% vs. 13%, P = 0.02, respectively), as well as with a lower LVEF both in the acute phase after infarction (35% vs. 54%, P < 0.001) and in the chronic phase (42% vs. 56%, P < 0.001), larger IS in the acute (32% vs. 15%, P < 0.001) and in the chronic phases (26% vs. 11%, P < 0.001), and larger left ventricular volumes (119 ± 20 vs. 98 ± 14, P = 0.003) by CMR. Univariable and multivariable Cox regression analysis results showed that patients with GSDMD concentrations ≧ median (13 ng/L) had a higher incidence of MACE (P < 0.05).
Conclusions: High GSDMD concentrations in STEMI patients are associated with microvascular injury (including MVO and IMH), which is a powerful MACE predictor. Nevertheless, the therapeutic implications of this relation need further research.
Keywords: GSDMD; IMH; MVO; ST-segment elevation myocardial infarction; magnetic resonance imaging; microvascular dysfunction.
© 2023 Sun, Wang, Cui, Wang, Zhao, Lu, Yang, Dong and Chu.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures

Similar articles
-
Microvascular obstruction extent predicts major adverse cardiovascular events in patients with acute myocardial infarction and preserved ejection fraction.Eur Radiol. 2019 May;29(5):2369-2377. doi: 10.1007/s00330-018-5895-z. Epub 2018 Dec 14. Eur Radiol. 2019. PMID: 30552479
-
Association of plasma interleukin-6 with infarct size, reperfusion injury, and adverse remodelling after ST-elevation myocardial infarction.Eur Heart J Acute Cardiovasc Care. 2022 Feb 8;11(2):113-123. doi: 10.1093/ehjacc/zuab110. Eur Heart J Acute Cardiovasc Care. 2022. PMID: 34849677 Clinical Trial.
-
Relationship between admission Q waves and microvascular injury in patients with ST-elevation myocardial infarction treated with primary percutaneous coronary intervention.Int J Cardiol. 2019 Dec 15;297:1-7. doi: 10.1016/j.ijcard.2019.10.009. Epub 2019 Oct 12. Int J Cardiol. 2019. PMID: 31629564
-
Cardiovascular magnetic resonance-derived intramyocardial hemorrhage after STEMI: Influence on long-term prognosis, adverse left ventricular remodeling and relationship with microvascular obstruction.Int J Cardiol. 2013 Sep 1;167(5):2047-54. doi: 10.1016/j.ijcard.2012.05.055. Epub 2012 Jun 9. Int J Cardiol. 2013. PMID: 22682700
-
Impact of Intramyocardial Hemorrhage on Clinical Outcomes in ST-Elevation Myocardial Infarction: A Systematic Review and Meta-analysis.J Soc Cardiovasc Angiogr Interv. 2022 Aug 26;1(6):100444. doi: 10.1016/j.jscai.2022.100444. eCollection 2022 Nov-Dec. J Soc Cardiovasc Angiogr Interv. 2022. PMID: 39132339 Free PMC article. Review.
References
-
- de Waha S, Patel M, Granger C, Ohman E, Maehara A, Eitel I, et al. Relationship between microvascular obstruction and adverse events following primary percutaneous coronary intervention for ST-segment elevation myocardial infarction: an individual patient data pooled analysis from seven randomized trials. Eur Heart J. (2017) 38(47):3502–10. 10.1093/eurheartj/ehx414 - DOI - PubMed
-
- Ghugre N, Pop M, Thomas R, Newbigging S, Qi X, Barry J, et al. Hemorrhage promotes inflammation and myocardial damage following acute myocardial infarction: insights from a novel preclinical model and cardiovascular magnetic resonance. J Cardiovasc Magn Reson. (2017) 19(1):50. 10.1186/s12968-017-0361-7 - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

