Trajectories of drug treatment and illicit opioid use in the AIDS Linked to the IntraVenous Experience cohort, 2014-2019
- PMID: 37429162
- PMCID: PMC10528295
- DOI: 10.1016/j.drugpo.2023.104120
Trajectories of drug treatment and illicit opioid use in the AIDS Linked to the IntraVenous Experience cohort, 2014-2019
Abstract
Background: Medication for opioid use disorder (MOUD) is an effective intervention to combat opioid use disorder and overdose, yet there is limited understanding of engagement in treatment over time in the community, contextualized by ongoing substance use. We aimed to identify concurrent trajectories of methadone prescriptions, buprenorphine prescriptions, and illicit opioid use among older adults with a history of injection drug use.
Methods: We used data on 887 participants from the AIDS Linked to the IntraVenous Experience cohort, who were engaged in the study in 2013 and attended ≥1 visit during follow-up (2014-2019). Outcomes were self-reported MOUD prescription and illicit opioid use in the last 6 months. To identify concurrent trajectories in all 3 outcomes, we used group-based multi-trajectory modeling. We examined participant characteristics, including sociodemographics, HIV status, and other substance use, overall and by cluster.
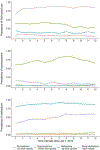
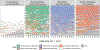
Results: We identified 4 trajectory clusters: (1) no MOUD and no illicit opioid use (43%); (2) buprenorphine and some illicit opioid use (11%); (3) methadone and no illicit opioid use (28%); and (4) some methadone and illicit opioid use (18%). While prevalence of each outcome was stable across time, transitions on/off treatment or on/off illicit opioid use occurred, with the rate of transition varying by cluster. The rate of transition was highest in Cluster 3 (0.74/person-year) and lowest in Cluster 1 (0.18/person-year). We saw differences in participant characteristics by cluster, including that the buprenorphine cluster had the highest proportion of people with HIV and participants who identified as non-Hispanic Black.
Conclusions: Most participants had discontinued illicit opioid use and were also not accessing MOUD. Trajectories defined by engagement with buprenorphine or methadone had distinct sociodemographic and behavioral characteristics, indicating that tailored interventions to expand access to both types of treatment are likely needed to reduce harms associated with untreated opioid use disorder.
Keywords: Buprenorphine; Longitudinal data; Medication for opioid use disorder; Methadone; Opioid use; Trajectory analysis.
Copyright © 2023 Elsevier B.V. All rights reserved.
Conflict of interest statement
Declarations of Interest The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Figures
Similar articles
-
Impact of fentanyl use on initiation and discontinuation of methadone and buprenorphine/naloxone among people with prescription-type opioid use disorder: secondary analysis of a Canadian treatment trial.Addiction. 2022 Oct;117(10):2662-2672. doi: 10.1111/add.15954. Epub 2022 Jun 17. Addiction. 2022. PMID: 35712892 Free PMC article. Clinical Trial.
-
Factors associated with retention on medications for opioid use disorder among a cohort of adults seeking treatment in the community.Addict Sci Clin Pract. 2022 Mar 7;17(1):15. doi: 10.1186/s13722-022-00299-1. Addict Sci Clin Pract. 2022. PMID: 35255967 Free PMC article.
-
Cardiac and mortality outcome differences between methadone, buprenorphine and naltrexone prescriptions in patients with an opioid use disorder.J Clin Psychol. 2023 Dec;79(12):2869-2883. doi: 10.1002/jclp.23582. Epub 2023 Aug 16. J Clin Psychol. 2023. PMID: 37584532
-
Maintenance medication for opiate addiction: the foundation of recovery.J Addict Dis. 2012;31(3):207-25. doi: 10.1080/10550887.2012.694598. J Addict Dis. 2012. PMID: 22873183 Free PMC article. Review.
-
Access to Medications for Opioid Use Disorder and Associated Factors Among Adolescents and Young Adults: A Systematic Review.JAMA Pediatr. 2022 Mar 1;176(3):304-311. doi: 10.1001/jamapediatrics.2021.4606. JAMA Pediatr. 2022. PMID: 34870707 Free PMC article.
Cited by
-
Longitudinal patterns of use of stimulants and opioids in the AIDS linked to the IntraVenous experience cohort, 2005-2019.Int J Drug Policy. 2024 Apr;126:104364. doi: 10.1016/j.drugpo.2024.104364. Epub 2024 Feb 25. Int J Drug Policy. 2024. PMID: 38408416 Free PMC article.
-
Drug treatment and support service utilization amidst the COVID-19 pandemic among people who inject drugs in Baltimore, Maryland: An interrupted time-series analysis, 2015-2022.Int J Drug Policy. 2025 Apr;138:104746. doi: 10.1016/j.drugpo.2025.104746. Epub 2025 Mar 3. Int J Drug Policy. 2025. PMID: 40037106
-
Association of inadequate sleep with mortality among persons who inject drugs.Sleep Health. 2024 Dec;10(6):651-657. doi: 10.1016/j.sleh.2024.07.008. Epub 2024 Sep 14. Sleep Health. 2024. PMID: 39278806
-
Structural and social changes due to the COVID-19 pandemic and their impact on engagement in substance use disorder treatment services: a qualitative study among people with a recent history of injection drug use in Baltimore, Maryland.Harm Reduct J. 2024 May 8;21(1):91. doi: 10.1186/s12954-024-01008-8. Harm Reduct J. 2024. PMID: 38720307 Free PMC article.
References
-
- Drug Overdose Deaths in the U.S. Top 100,000 Annually. Published November 17, 2021. Accessed November 7, 2022. https://www.cdc.gov/nchs/pressroom/nchs_press_releases/2021/20211117.htm
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

