Bilateral lung transplantation for pediatric pulmonary arterial hypertension: perioperative management and one-year follow-up
- PMID: 37441704
- PMCID: PMC10333590
- DOI: 10.3389/fcvm.2023.1193326
Bilateral lung transplantation for pediatric pulmonary arterial hypertension: perioperative management and one-year follow-up
Abstract
Background: Bilateral lung transplantation (LuTx) remains the only established treatment for children with end-stage pulmonary arterial hypertension (PAH). Although PAH is the second most common indication for LuTx, little is known about optimal perioperative management and midterm clinical outcomes.
Methods: Prospective observational study on consecutive children with PAH who underwent LuTx with scheduled postoperative VA-ECMO support at Hannover Medical School from December 2013 to June 2020.
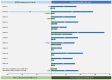
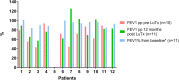
Results: Twelve patients with PAH underwent LuTx (mean age 11.9 years; age range 1.9-17.8). Underlying diagnoses included idiopathic (n = 4) or heritable PAH (n = 4), PAH associated with congenital heart disease (n = 2), pulmonary veno-occlusive disease (n = 1), and pulmonary capillary hemangiomatosis (n = 1). The mean waiting time was 58.5 days (range 1-220d). Three patients were bridged to LuTx on VA-ECMO. Intraoperative VA-ECMO/cardiopulmonary bypass was applied and VA-ECMO was continued postoperatively in all patients (mean ECMO-duration 185 h; range 73-363 h; early extubation). The median postoperative ventilation time was 28 h (range 17-145 h). Echocardiographic conventional and strain analysis showed that 12 months after LuTx, all patients had normal biventricular systolic function. All PAH patients are alive 2 years after LuTx (median follow-up 53 months, range 26-104 months).
Conclusion: LuTx in children with end-stage PAH resulted in excellent midterm outcomes (100% survival 2 years post-LuTx). Postoperative VA-ECMO facilitates early extubation with rapid gain of allograft function and sustained biventricular reverse-remodeling and systolic function after RV pressure unloading and LV volume loading.
Keywords: awake ECMO; children; extracorporeal membrane oxygenation (ECMO); lung transplantation; pediatric; pulmonary arterial hypertension.
© 2023 Jack, Carlens, Diekmann, Hasan, Chouvarine, Schwerk, Müller, Wieland, Tudorache, Warnecke, Avsar, Horke, Ius, Bobylev and Hansmann.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest. The handling editor SM declared a shared committee working group lung transplantation with the author FI at the time of review.
Figures


Similar articles
-
Full recovery of right ventricular systolic function in children undergoing bilateral lung transplantation for severe PAH.J Heart Lung Transplant. 2022 Feb;41(2):187-198. doi: 10.1016/j.healun.2021.10.014. Epub 2021 Oct 29. J Heart Lung Transplant. 2022. PMID: 34955331
-
Transient perioperative inflammation following lung transplantation and major thoracic surgery with elective extracorporeal support: a prospective observational study.Ann Transl Med. 2021 Mar;9(5):385. doi: 10.21037/atm-20-4771. Ann Transl Med. 2021. PMID: 33842606 Free PMC article.
-
Bilateral lung transplantation with intra- and postoperatively prolonged ECMO support in patients with pulmonary hypertension.Eur J Cardiothorac Surg. 2002 May;21(5):858-63. doi: 10.1016/s1010-7940(02)00058-1. Eur J Cardiothorac Surg. 2002. PMID: 12062275
-
Outcome of Extracorporeal Membrane Oxygenation as a Bridge To Lung Transplantation: An Institutional Experience and Literature Review.Transplantation. 2015 Aug;99(8):1667-71. doi: 10.1097/TP.0000000000000653. Transplantation. 2015. PMID: 26308302 Review.
-
A Review of Pulmonary Arterial Hypertension Treatment in Extracorporeal Membrane Oxygenation: A Case Series of Adult Patients.J Cardiovasc Pharmacol Ther. 2022 Jan-Dec;27:10742484211069005. doi: 10.1177/10742484211069005. J Cardiovasc Pharmacol Ther. 2022. PMID: 35006031 Review.
Cited by
-
Post-operative management of children after lung transplantation.JHLT Open. 2025 May 27;9:100301. doi: 10.1016/j.jhlto.2025.100301. eCollection 2025 Aug. JHLT Open. 2025. PMID: 40606299 Free PMC article.
-
Interventional Strategies for Children with Progressive Pulmonary Hypertension Despite Optimal Therapy: An Official American Thoracic Society Clinical Practice Guideline.Am J Respir Crit Care Med. 2025 Feb;211(2):157-173. doi: 10.1164/rccm.202410-1901ST. Am J Respir Crit Care Med. 2025. PMID: 39531626 Free PMC article.
References
-
- Hansmann G, Koestenberger M, Alastalo TP, Apitz C, Austin ED, Bonnet D, et al. 2019 updated consensus statement on the diagnosis and treatment of pediatric pulmonary hypertension: the European pediatric pulmonary vascular disease network (EPPVDN), endorsed by AEPC, ESPR and ISHLT. J Heart Lung Transplant. (2019) 38:879–901. 10.1016/j.healun.2019.06.022 - DOI - PubMed
LinkOut - more resources
Full Text Sources

