Ocular Involvement of Granulomatosis with Polyangiitis
- PMID: 37445483
- PMCID: PMC10342598
- DOI: 10.3390/jcm12134448
Ocular Involvement of Granulomatosis with Polyangiitis
Abstract
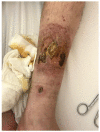
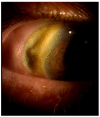
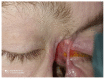
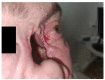
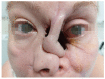
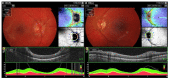
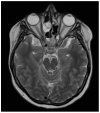
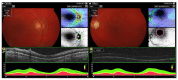
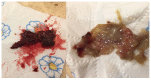
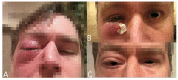
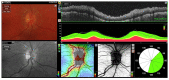
Granulomatosis with polyangiitis (GPA), formerly referred to as Wegener's disease, is a form of ANCA-associated vasculitis. It manifests mainly in the kidneys and the upper respiratory tract, but ocular involvement is not uncommon. In this article, four cases with ocular manifestations are presented with comprehensive photographic documentation. We describe the way to proper diagnosis, which may be long, the possible treatment, and the final outcomes. Our patients had the following ocular manifestations of GPA: retinal vasculitis, anterior necrotizing scleritis, medial orbital wall and orbital floor erosion with middle face deformation, compressive optic neuropathy due to retrobulbar inflammatory mass, and the abscess of the eyelids, inflammatory intraorbital mass causing exophthalmos and diplopia. This manuscript includes the description of severe forms of GPA, the initial signs and symptoms, relapses, and difficulties in achieving remission. The extraocular involvement is described with diagnostic modalities and laboratory findings. One of the reported cases was diagnosed by an ophthalmologist on the basis of ocular symptoms in the early stages of the disease. Our outcomes are compared with those discussed in the literature.
Keywords: ANCA; GPA; GPA ocular symptoms; Wegener’s disease; vasculitis.
Conflict of interest statement
No conflict of interest to declare.
Figures










Similar articles
-
A rare case report of polyangiitis overlap syndrome: granulomatosis with polyangiitis and eosinophilic granulomatosis with polyangiitis.BMC Pulm Med. 2018 Nov 29;18(1):181. doi: 10.1186/s12890-018-0733-2. BMC Pulm Med. 2018. PMID: 30497438 Free PMC article. Review.
-
Exophthalmos as a presenting manifestation of limited Wegener's granulomatosis in a patient with prior graves' disease.Clin Med Case Rep. 2009 Jun 30;2:35-7. doi: 10.4137/ccrep.s731. eCollection 2009. Clin Med Case Rep. 2009. PMID: 24179371 Free PMC article.
-
Wegener's granulomatosis with orbital involvement: case report and literature review.Rom J Ophthalmol. 2021 Jan-Mar;65(1):93-97. doi: 10.22336/rjo.2021.19. Rom J Ophthalmol. 2021. PMID: 33817443 Free PMC article. Review.
-
Clinic manifestations in granulomatosis with polyangiitis.Int J Immunopathol Pharmacol. 2016 Jun;29(2):151-9. doi: 10.1177/0394632015617063. Epub 2015 Dec 18. Int J Immunopathol Pharmacol. 2016. PMID: 26684637 Free PMC article. Review.
-
Ocular Manifestations of Granulomatosis with Polyangiitis.Cesk Slov Oftalmol. 2019 Spring;74(5):167-174. doi: 10.31348/2018/5/1. Cesk Slov Oftalmol. 2019. PMID: 31234629 English.
Cited by
-
[Peripheral ulcerative keratitis with necrotizing scleritis, manifestation of granulomatosis with polyangiitis].Rev Med Inst Mex Seguro Soc. 2025 Mar 3;63(2):e6015. doi: 10.5281/zenodo.14617182. Rev Med Inst Mex Seguro Soc. 2025. PMID: 40279461 Free PMC article. Spanish.
-
Granulomatosis with Polyangiitis Discovered Because of Repeated Upper Eyelid Swelling.Medicina (Kaunas). 2024 Sep 23;60(9):1555. doi: 10.3390/medicina60091555. Medicina (Kaunas). 2024. PMID: 39336596 Free PMC article.
-
Eosinophilic Granulomatosis With Polyangiitis Presenting as Bilateral Orbital Inflammation.Cureus. 2025 Apr 28;17(4):e83131. doi: 10.7759/cureus.83131. eCollection 2025 Apr. Cureus. 2025. PMID: 40438859 Free PMC article.
References
-
- Miloslavsky E.M., Lu N., Unizony S., Choi H.K., Merkel P.A., Seo P., Spiera R., Langford C.A., Hoffman G.S., Kallenberg C.G.M., et al. Myeloperoxidase-Antineutrophil Cytoplasmic Antibody (ANCA)-Positive and ANCA-Negative Patients with Granulomatosis with Polyangiitis (Wegener’s): Distinct Patient Subsets. Arthritis Rheumatol. 2016;68:2945–2952. doi: 10.1002/ART.39812. - DOI - PMC - PubMed
-
- Finkielman J.D., Lee A.S., Hummel A.M., Viss M.A., Jacob G.L., Homburger H.A., Peikert T., Hoffman G.S., Merkel P.A., Spiera R., et al. ANCA Are Detectable in Nearly All Patients with Active Severe Wegener’s Granulomatosis. Am. J. Med. 2007;120:643.e9–643.e14. doi: 10.1016/j.amjmed.2006.08.016. - DOI - PubMed
-
- Eye Involvement in ANCA Positive Vasculitis-PubMed. [(accessed on 7 May 2023)]; Available online: https://pubmed.ncbi.nlm.nih.gov/32292850/
LinkOut - more resources
Full Text Sources

