Cervical Spinal Epidural Abscess: Diagnosis, Treatment, and Outcomes: A Case Series and a Literature Review
- PMID: 37445544
- PMCID: PMC10342465
- DOI: 10.3390/jcm12134509
Cervical Spinal Epidural Abscess: Diagnosis, Treatment, and Outcomes: A Case Series and a Literature Review
Abstract
Although recent diagnostic and management methods have improved the prognosis of cervical epidural abscesses, morbidity and mortality remain significant. The purpose of our study is to define the clinical presentation of cervical spinal epidural abscess, to determine the early clinical outcome of surgical treatment, and to identify the most effective diagnostic and treatment approaches. Additionally, we analyzed studies regarding cervical epidural abscesses and performed a review of the literature. In this study, four patients with spinal epidural abscess were included. There were three men and one woman with a mean age of 53 years. Three patients presented with motor deficits, and one patient was diagnosed incidentally through spinal imaging. All the patients had fever, and blood cultures were positive. Staphylococcus aureus was the most common organism cultured from abscesses. All patients underwent a surgical procedure, and three patients recovered their normal neurological functions, but one remained with mild neurological disability that was resolved two years postoperatively. The mean follow-up period was 12 months, and no deaths occurred in this series. Furthermore, we identified 85 studies in the literature review and extracted data regarding the diagnosis and management of these patients. The timely detection and effective management of this condition are essential for minimizing its associated morbidity and mortality.
Keywords: cervical spinal epidural abscess; outcome; surgery; treatment.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
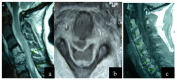

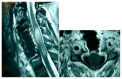
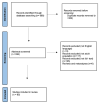
References
LinkOut - more resources
Full Text Sources

