Simplified soft tissue coverage of the distal lower extremity: The reverse sural flap
- PMID: 37448567
- PMCID: PMC10337849
- DOI: 10.1097/OI9.0000000000000235
Simplified soft tissue coverage of the distal lower extremity: The reverse sural flap
Abstract
Soft tissue defects involving the distal lower extremity present challenging problems for orthopaedic surgeons to manage. Historically, wounds not amenable to primary closure have necessitated assistance from multidisciplinary teams using plastic surgeons to obtain adequate soft tissue coverage through rotational flap or free tissue transfer procedures. Techniques related to soft tissue rearrangement and local rotational flap coverage have advanced over the years with a growing knowledge of local anatomy and vasculature. The reverse sural flap may be performed to cover soft tissue defects within 10 cm of the foot or ankle region, negating the need for microvascular intervention. The simplistic nature of the reverse sural flap is appealing to orthopaedic surgeons as a means to provide timely patient care without additional support because it does not require microvasculature work or the need for intraoperative microscopes and has been popularized among orthopaedic trauma surgeons as a necessary tool to possess. Here, we discuss the reverse sural flap to include history, relevant anatomy, clinical indications, and a description of the technique for application.
Keywords: coverage; flap; reverse; rotational; soft; sural; tissue.
Copyright © 2023 The Authors. Published by Wolters Kluwer Health, Inc. on behalf of the Orthopaedic Trauma Association.
Conflict of interest statement
Dr. J. A. Blair is a consultant for Stryker, Inc., Smith & Nephew, Inc, Integra Lifesciences, Corporation, and NuVasive Specialized Orthopaedics. The remaining authors have no relevant disclosures.
Figures
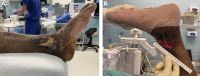
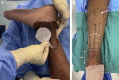
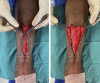

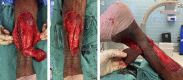
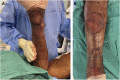
References
-
- Pincus D, Byrne JP, Nathens AB, et al. Delay in flap coverage past 7 days increases complications for open tibia fractures: a cohort study of 140 North American trauma centers. J Orthop Trauma. 2019;33:161–168. - PubMed
-
- Gopal S, Majumder S, Batchelor AG, et al. Fix and flap: the radical orthopaedic and plastic treatment of severe open fractures of the tibia. J Bone Joint Surg Br. 2000;82:959–966. - PubMed
-
- Akhtar S, Hameed A. Versatility of the sural fasciocutaneous flap in the coverage of lower third leg and hind foot defects. J Plast Reconstr Aesthet Surg. 2006;59:839–845. - PubMed
-
- Blair JA, Puneky GA, Dickerson TE, et al. Posttraumatic soft tissue coverage of the lower leg for the orthopedic surgeon. Orthop Clin North Am. 2022;53:297–310. - PubMed
LinkOut - more resources
Full Text Sources
