The age profile of respiratory syncytial virus burden in preschool children of low- and middle-income countries: A semi-parametric, meta-regression approach
- PMID: 37459352
- PMCID: PMC10389726
- DOI: 10.1371/journal.pmed.1004250
The age profile of respiratory syncytial virus burden in preschool children of low- and middle-income countries: A semi-parametric, meta-regression approach
Abstract
Background: Respiratory syncytial virus (RSV) infections are among the primary causes of death for children under 5 years of age worldwide. A notable challenge with many of the upcoming prophylactic interventions against RSV is their short duration of protection, making the age profile of key interest to the design of prevention strategies.
Methods and findings: We leverage the RSV data collected on cases, hospitalizations, and deaths in a systematic review in combination with flexible generalized additive mixed models (GAMMs) to characterize the age burden of RSV incidence, hospitalization, and hospital-based case fatality rate (hCFR). Due to the flexible nature of GAMMs, we estimate the peak, median, and mean incidence of infection to inform discussions on the ideal "window of protection" of prophylactic interventions. In a secondary analysis, we reestimate the burden of RSV in all low- and middle-income countries. The peak age of community-based incidence is 4.8 months, and the mean and median age of infection is 18.9 and 14.7 months, respectively. Estimating the age profile using the incidence coming from hospital-based studies yields a slightly younger age profile, in which the peak age of infection is 2.6 months and the mean and median age of infection are 15.8 and 11.6 months, respectively. More severe outcomes, such as hospitalization and in-hospital death have a younger age profile. Children under 6 months of age constitute 10% of the population under 5 years of age but bear 20% to 29% of cases, 28% to 39% of hospitalizations, and 38% to 50% of deaths. On an average year, we estimate 28.23 to 31.34 million cases of RSV, between 2.95 to 3.35 million hospitalizations, and 16,835 to 19,909 in-hospital deaths in low, lower- and upper middle-income countries. In addition, we estimate 17,254 to 23,875 deaths in the community, for a total of 34,114 to 46,485 deaths. Globally, evidence shows that community-based incidence may differ by World Bank Income Group, but not hospital-based incidence, probability of hospitalization, or the probability of in-hospital death (p ≤ 0.01, p = 1, p = 0.86, 0.63, respectively). Our study is limited mainly due to the sparsity of the data, especially for low-income countries (LICs). The lack of information for some populations makes detecting heterogeneity between income groups difficult, and differences in access to care may impact the reported burden.
Conclusions: We have demonstrated an approach to synthesize information on RSV outcomes in a statistically principled manner, and we estimate that the age profile of RSV burden depends on whether information on incidence is collected in hospitals or in the community. Our results suggest that the ideal prophylactic strategy may require multiple products to avert the risk among preschool children.
Copyright: © 2023 Antillón et al. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Conflict of interest statement
I have read the journal’s policy and the authors of this manuscript have the following competing interests: LW received grants from Research Foundation Flanders (FWO) during the conduct of the study and fees from Pfizer outside the submitted work for discussions on economic evaluation, for a total of <€3000 combined, fully paid directly to the University of Antwerp. PB reports a grant from the Respiratory Syncytial Virus Consortium in Europe (RESCEU), Innovative Medicines Initiative 2 of the European Commission, Joint Undertaking under grant agreement No 116019, during the conduct of the study; and outside the submitted work he reports grants from Pfizer, GSK, Merck and the Innovative Medicines Initiative 2 of the European Commission (N° 101034339 project PROMISE: Preparing for RSV immunisation and surveillance in Europe) as well as consultancy fees.
Figures
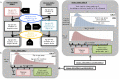






References
-
- O’Brien KL, Baggett HC, Brooks WA, Feikin DR, Hammitt LL, Higdon MM, et al. Causes of severe pneumonia requiring hospital admission in children without HIV infection from Africa and Asia: the PERCH multi-country case-control study. Lancet. 2019;394(10200):757–779. doi: 10.1016/S0140-6736(19)30721-4 - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

