Comparison of remimazolam-remifentanil and propofol-remifentanil during laparoscopic cholecystectomy
- PMID: 37468208
- PMCID: PMC10410549
- DOI: 10.17085/apm.22252
Comparison of remimazolam-remifentanil and propofol-remifentanil during laparoscopic cholecystectomy
Abstract
Background: Remimazolam is a novel benzodiazepine with fast onset and short half-life. We compared the effects of remimazolam and propofol on recovery profiles for general anesthesia in patients undergoing laparoscopic cholecystectomy.
Methods: We randomly assigned 108 patients to either a remimazolam (n=54) or propofol (n=54) group. Remimazolam and propofol were used for induction and maintanance of anesthesia. Following anesthesia, we recorded the time until an Aldrete score of 9 was achieved as the primary surrogate marker of complete recovery. The time to reach a Modified Observer's Assessment of Alertness/Sedation (MOAA/S) score of 2 and the time from the end of anesthesia to eye opening time, recovery time of orientation, time to spontaneous breathing, extubation time, and the time required for analgesics were measured. Heart rate, blood pressure, and bispectral index were assessed before, during, and after pneumoperitoneum.
Results: We included 101 patients in the analysis. In the remimazolam group, it took longer to reach an Aldrete score of 9 after the drug infusion ended (P = 0.031). There was no difference in the time to reach MOAA/S 2 between the two groups. The time to eye opening, recovery time of orientation, and time required for analgesics were longer and heart rate was higher in the remimazolam group. Neither blood pressure, nor extubation time differed between groups.
Conclusions: Remimazolam and propofol provided safe induction and maintenance of anesthesia in patients undergoing laparoscopic cholecystectomy. The recovery time from anesthesia was longer than that with propofol. Fewer hemodynamic changes were observed with remimazolam, but further studies are needed.
Keywords: Benzodiazepine; Cholecystectomy; Laparoscopy; Propofol; Remifentanil.
Conflict of interest statement
No potential conflict of interest relevant to this article was reported.
Figures


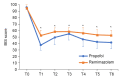
References
-
- Juckenhöfel S, Feisel C, Schmitt HJ, Biedler A. TIVA with propofol-remifentanil or balanced anesthesia with sevoflurane-fentanyl in laparoscopic operations. Hemodynamics, awakening and adverse effects. Anaesthesist. 1999;48:807–12. - PubMed
-
- Zhang Y, Shan GJ, Zhang YX, Cao SJ, Zhu SN, Li HJ, et al. First Study of Perioperative Organ Protection (SPOP1) investigators Propofolcomparedwithsevofluranegeneralanaesthesiaisassociatedwithdecreaseddelayedneurocognitiverecoveryinolderadults. Br J Anaesth. 2018;121:595–604. - PubMed
LinkOut - more resources
Full Text Sources

