Multidrug-Resistant Bacterial Colonization and Infections in Large Retrospective Cohort of Mechanically Ventilated COVID-19 Patients1
- PMID: 37486196
- PMCID: PMC10370845
- DOI: 10.3201/eid2908.230115
Multidrug-Resistant Bacterial Colonization and Infections in Large Retrospective Cohort of Mechanically Ventilated COVID-19 Patients1
Abstract
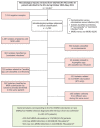
Few data are available on incidence of multidrug-resistant organism (MDRO) colonization and infections in mechanically ventilated patients, particularly during the COVID-19 pandemic. We retrospectively evaluated all patients admitted to the COVID-19 intensive care unit (ICU) of Hub Hospital in Milan, Italy, during October 2020‒May 2021. Microbiologic surveillance was standardized with active screening at admission and weekly during ICU stay. Of 435 patients, 88 (20.2%) had MDROs isolated ≤48 h after admission. Of the remaining patients, MDRO colonization was diagnosed in 173 (51.2%), MDRO infections in 95 (28.1%), and non-MDRO infections in 212 (62.7%). Non-MDRO infections occurred earlier than MDRO infections (6 days vs. 10 days; p<0.001). Previous exposure to antimicrobial drugs within the ICU was higher in MDRO patients than in non-MDRO patients (116/197 [58.9%] vs. 18/140 [12.9%]; p<0.001). Our findings might serve as warnings for future respiratory viral pandemics and call for increased measures of antimicrobial stewardship and infection control.
Keywords: COVID-19; MDR; MDRO; SARS-CoV-2; antimicrobial resistance; antimicrobial stewardship; bacteria; colonization; incidence rate; infections; intensive care unit; large retrospective cohort; mechanically ventilated patients; multidrug resistant; multidrug-resistant bacteria; multidrug-resistant organism; respiratory infections; zoonoses.
Figures


References
-
- Russell CD, Fairfield CJ, Drake TM, Turtle L, Seaton RA, Wootton DG, et al. ; ISARIC4C investigators. Co-infections, secondary infections, and antimicrobial use in patients hospitalised with COVID-19 during the first pandemic wave from the ISARIC WHO CCP-UK study: a multicentre, prospective cohort study. Lancet Microbe. 2021;2:e354–65. 10.1016/S2666-5247(21)00090-2 - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

