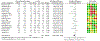Psychological treatments for the management of pain after musculoskeletal injury: a systematic review and meta-analysis
- PMID: 37490624
- PMCID: PMC10808265
- DOI: 10.1097/j.pain.0000000000002991
Psychological treatments for the management of pain after musculoskeletal injury: a systematic review and meta-analysis
Abstract
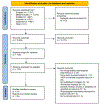
Musculoskeletal injury is a leading cause of pain and disability worldwide; 35% to 75% of people experience persistent pain for months and years after injury. Psychological treatments can reduce pain, functional impairment, and psychological distress but are not widely used after injury. This systematic review and meta-analysis (PROSPERO ID: CRD42021236807) aimed to synthesize the literature testing psychological treatments for pain after musculoskeletal injury. We searched EMBASE, MEDLINE, PubMed, PsycINFO, and CENTRAL from inception to May 2022. We extracted participant, treatment, and injury characteristics and primary (eg, pain intensity, functional impairment, depression, anxiety, and PTSD symptoms) and secondary (treatment feasibility and acceptability) outcomes. Twenty-four randomized controlled trials (N = 1966) were included. Immediately posttreatment, people who received psychological treatments (versus any control) reported lower pain intensity (standardized mean differences [SMD] = -0.25, 95% confidence interval [-0.49, -0.02]), functional impairment (SMD = -0.32 [-0.55, -0.09]), and symptoms of depression (SMD = -0.46 [-0.64, -0.29]), anxiety (SMD = -0.34 [-0.65, -0.04]), and PTSD (SMD = -0.43 [-0.70, -0.15]); at 6-month follow-up, only depression symptoms were significantly lower. Included trials varied widely in treatment and injury characteristics. The certainty of evidence was low or very low for most effects and heterogeneity moderate to substantial. Most studies had risk of bias domains judged to be high or unclear. Owing to very low certainty of results, we are unsure whether psychological therapies reduce pain and functional impairment after musculoskeletal injury; they may result in improved depression immediately posttreatment and at follow-up. More research is needed to identify treatments that result in enduring effects.
Copyright © 2023 International Association for the Study of Pain.
Conflict of interest statement
Figures
References
-
- Achterberg J, Kenner C, Casey D. Behavioral strategies for the reduction of pain and anxiety associated with orthopedic trauma. Biofeedback and self-regulation 1989;14(2):101–114. - PubMed
-
- Andersen TE, Ravn SL, Armfield N, Maujean A, Requena SS, Sterling M. Trauma-focused cognitive behavioural therapy and exercise for chronic whiplash with comorbid posttraumatic stress disorder: a randomised controlled trial. Pain 2021;162(4):1221–1232. - PubMed
-
- Angst F, Francoise G, Verra M, Lehmann S, Jenni W, Aeschlimann A. Interdisciplinary rehabilitation after whiplash injury: an observational prospective outcome study. Journal of rehabilitation medicine 2010;42(4):350–356. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical