High-performing primary care clinics across high-need, high-cost Medicare populations
- PMID: 37491105
- PMCID: PMC10373721
- DOI: 10.1136/bmjoq-2023-002271
High-performing primary care clinics across high-need, high-cost Medicare populations
Abstract
Background: To reduce spending and improve quality, some primary care clinics in the USA have focused on high-need, high-cost (HNHC) Medicare beneficiaries, which include clinically distinct subpopulations: older adults with frailty, adults under 65 years with disability and beneficiaries with major complex chronic conditions. Nationally, the extent to which primary care clinics are high-performing 'Bright Spots'-clinics that achieve favourable outcomes at lower costs across HNHC beneficiary subpopulations-is not known.
Objective: To determine the prevalence of primary care clinics that perform highly on commonly used cost or quality measures for HNHC subpopulations.
Design and participants: Cross-sectional study using Medicare claims data from 2014 to 2015.
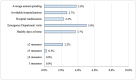
Main measures: Annual spending, avoidable hospitalisations for ambulatory care-sensitive conditions, treat-and-release emergency department visits, all-cause 30-day unplanned hospital readmission rates and healthy days at home. Clinics were high performing when they ranked in the top quartile of performance for ≥4 measures for an HNHC subpopulation. 'Bright Spot' clinics were in the top quartile of performance for ≥4 measures across all the HNHC subpopulations.
Key results: A total of 2770 primary care clinics cared for at least 10 beneficiaries from each of the three HNHC subpopulations (adults under 65 with disability, older adults with frailty and beneficiaries with major complex chronic conditions). Less than 4% of clinics were high performing for each HNHC subpopulation; <0.5% of clinics were in the top quartile for all five measures for a given subpopulation. No clinics met the definition of a primary care 'Bright Spot'.
Conclusions: High-performing primary care clinics that achieved favourable health outcomes or lower costs across subpopulations of HNHC beneficiaries in the Medicare programme in 2015 were rare. Efforts are needed to support primary care clinics in providing optimal care to HNHC subpopulations.
Keywords: GENERAL PRACTICE; Health policy; Health services research; Healthcare quality improvement; PRIMARY CARE.
© Author(s) (or their employer(s)) 2023. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ.
Conflict of interest statement
Competing interests: ALB reports previous service as the Special Advisor to the US Surgeon General at the Department of Health and Human Services in 2021 and prior employment with Aledade, all unrelated to this article. JF reports grants for other work not related to this study from the Commonwealth Fund, Robert Wood Johnson Foundation, Arnold Ventures and the National Institute on Aging. He has also received a research consultant contract from Humana not related to this work.
Figures
References
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous
