Effects of synovial macrophages in osteoarthritis
- PMID: 37492583
- PMCID: PMC10364050
- DOI: 10.3389/fimmu.2023.1164137
Effects of synovial macrophages in osteoarthritis
Abstract
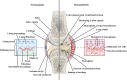
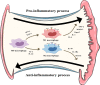
Osteoarthritis (OA) is a common degenerative disease in mammals. However, its pathogenesis remains unclear. Studies indicate that OA is not only an aging process that but also an inflammation-related disease. Synovitis is closely related to the progression of OA, and synovial macrophages are crucial participants in synovitis. Instead of being a homogeneous population, macrophages are polarized into M1 or M2 subtypes in OA synovial tissues. Polarization is highly associated with OA severity. However, the M1/M2 ratio cannot be the only factor in OA prognosis because intermediate stages of macrophages also exist. To better understand the mechanism of this heterogeneous disease, OA subtypes of synovial macrophages classified by gene expression were examined. Synovial macrophages do not act alone; they interact with surrounding cells such as synovial fibroblasts, osteoclasts, chondrocytes, lymphocytes and even adipose cells through a paracrine approach to exacerbate OA. Treatments targeting synovial macrophages and their polarization are effective in relieving pain and protecting cartilage during OA development. In this review, we describe how synovial macrophages and their different polarization states influence the progression of OA. We summarize the current knowledge of the interactions between macrophages and other joint cells and examine the current research on new medications targeting synovial macrophages.
Keywords: macrophages; osteoarthritis; polarization; review; synovial; treatment.
Copyright © 2023 Zhao, Ruan, Nie, Ye and Li.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures

References
-
- Hiligsmann M, Cooper C, Arden N, Boers M, Branco JC, Luisa Brandi M, et al. Health economics in the field of osteoarthritis: an expert's consensus paper from the European society for clinical and economic aspects of osteoporosis and osteoarthritis (ESCEO). Semin Arthritis Rheumatol (2013) 43(3):303–13. doi: 10.1016/j.semarthrit.2013.07.003 - DOI - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

