Advances in the Diagnosis and Management of Achalasia and Achalasia-Like Syndromes: Insights From HRM and FLIP
- PMID: 37503535
- PMCID: PMC10373628
- DOI: 10.1016/j.gastha.2023.02.001
Advances in the Diagnosis and Management of Achalasia and Achalasia-Like Syndromes: Insights From HRM and FLIP
Abstract
High-resolution manometry, Chicago Classification v4.0, the functional lumen imaging probe, Panometry, and peroral endoscopic myotomy (POEM) are all now integral parts of the landscape for managing achalasia or, more precisely, achalasia-like syndromes. This narrative review examines the impact of these innovations on the management of achalasia-like syndromes. High-resolution manometry was the disruptive technology that prompted the paradigm shift to thinking of motility disorders as patterns of obstructive physiology involving the esophagogastric junction and/or the distal esophagus rather than as siloed entities. An early observation was that the cardinal feature of achalasia-impaired lower esophageal sphincter relaxation-can occur in several subtypes: without peristalsis, with pan-esophageal pressurization, with premature (spastic) distal esophageal contractions, or even with preserved peristalsis (esophagogastric junction outlet obstruction). Furthermore, there being no biomarker for achalasia, no manometric pattern is perfectly sensitive or specific for 'achalasia' and there is also no 'gold standard' for the diagnosis. Consequently, complimentary physiological testing with a timed barium esophagram or functional lumen imaging probe are employed both to improve the detection of patients likely to respond to treatments for 'achalasia' and to characterize other syndromes also likely to benefit from achalasia therapies. These findings have become particularly relevant with the development of a minimally invasive technique for performing a tailored esophageal myotomy, POEM. Now and in the future, optimal achalasia management is to render treatment in a phenotype-specific manner, that is, POEM calibrated in a patient-specific manner for obstructive physiology including the distal esophagus and more conservative strategies such as a short POEM or pneumatic dilation for obstructive physiology limited to the lower esophageal sphincter.
Keywords: Achalasia; Dysphagia; Esophagus; Functional lumen imaging probe; Manometry.
Conflict of interest statement
Conflicts of Interest: These authors report the following: John E. Pandolfino, Peter J. Kahrilas, and Northwestern University hold shared intellectual property rights and ownership surrounding FLIP Panometry systems, methods, and apparatus with Medtronic Inc. Peter J. Kahrilas: Ironwood (Consulting); Reckitt (Consulting), Phathom (consulting). Dustin A. Carlson: Medtronic (Speaking, Consulting); Phathom Pharmaceuticals (Consulting). John E. Pandolfino: Sandhill Scientific/Diversatek (Consulting, Speaking, Grant), Takeda (Speaking), Astra Zeneca (Speaking), Medtronic (Speaking, Consulting, Patent, License), Torax (Speaking, Consulting), Ironwood (Consulting).
Figures
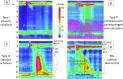



References
-
- Kuipers T., Ponds F.A., Fockens P., et al. Peroral endoscopic myotomy vs pneumatic dilation in treatment-naive patients with achalasia: long-term results of a randomized controlled trial. Lancet Gastroenterol Hepatol. 2022;7(12):1103–1111. - PubMed
-
- Werner Y.B., Hakanson B., Martinek J., et al. Endoscopic or surgical myotomy in patients with idiopathic achalasia. N Engl J Med. 2019;381:2219–2229. - PubMed
-
- Andolfi C., Fisichella P.M. Meta-analysis of clinical outcome after treatment for achalasia based on manometric subtypes. Br J Surg. 2019;106(4):332–341. - PubMed
-
- Knowles T.B., Jackson A.S., Chang S.C., et al. Changes in distensibility index during an incremental POEM myotomy. J Gastrointest Surg. 2022;26(6):1140–1146. - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources

