Increased small extracellular vesicle levels and decreased miR-126 levels associated with atrial fibrillation and coexisting diabetes mellitus
- PMID: 37503820
- PMCID: PMC10642338
- DOI: 10.1002/clc.24115
Increased small extracellular vesicle levels and decreased miR-126 levels associated with atrial fibrillation and coexisting diabetes mellitus
Abstract
Background: Atrial fibrillation (AF) is the most prevalent cardiac arrhythmia. Diabetes mellitus (DM) is one of the risk factors for the development of stroke and thromboembolism in patients with AF. Early identification may reduce the incidence of complications and mortality in AF patients.
Hypothesis: AF patients with DM have different pattern of small extracellular vesicle (sEV) levels and sEV-derived microRNA (miRNA) expression compared with those without DM.
Methods: We compared sEV levels and sEV-miRNA expression in plasma from AF patients with and without DM using nanoparticle tracking analysis and droplet digital polymerase chain reaction, respectively.
Results: We observed a significant increase in total sEV levels (p = .004) and a significant decrease in sEV-miR-126 level (p = .004) in AF patients with DM. Multivariate logistic regression analysis revealed a positive association between total sEV levels and AF with DM (p = .019), and a negative association between sEV-miR-126 level and AF with DM (p = .031). The combination of clinical data, total sEVs, and sEV-miR-126 level had an area under the curve of 0.968 (p < .0001) for discriminating AF with DM, which was shown to be significantly better than clinical data analysis alone (p = .0368).
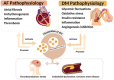
Conclusions: These results suggest that an increased level of total sEV and a decreased sEV-miR-126 level may play a potential role in the pathophysiology and complications of AF with DM, especially endothelial dysfunction, and can be considered as an applied biomarker for distinguishing between AF with and without DM.
Keywords: atrial fibrillation; diabetes mellitus; microRNAs; small extracellular vesicles.
© 2023 The Authors. Clinical Cardiology published by Wiley Periodicals LLC.
Conflict of interest statement
The authors declare no conflict of interest.
Figures




Similar articles
-
Diabetes mellitus as risk factor for atrial fibrillation hospitalization: Incidence and outcomes over nine years in a region of Northern Italy.Diabetes Res Clin Pract. 2015 Sep;109(3):476-84. doi: 10.1016/j.diabres.2015.06.006. Epub 2015 Jul 17. Diabetes Res Clin Pract. 2015. PMID: 26220013
-
Increased expression of six-large extracellular vesicle-derived miRNAs signature for nonvalvular atrial fibrillation.J Transl Med. 2022 Jan 3;20(1):4. doi: 10.1186/s12967-021-03213-6. J Transl Med. 2022. PMID: 34980172 Free PMC article.
-
Serum outperforms plasma in small extracellular vesicle microRNA biomarker studies of adenocarcinoma of the esophagus.World J Gastroenterol. 2020 May 28;26(20):2570-2583. doi: 10.3748/wjg.v26.i20.2570. World J Gastroenterol. 2020. PMID: 32523312 Free PMC article.
-
The complex interplay between diabetes mellitus and atrial fibrillation.Expert Rev Cardiovasc Ther. 2022 Sep;20(9):707-717. doi: 10.1080/14779072.2022.2115357. Epub 2022 Aug 25. Expert Rev Cardiovasc Ther. 2022. PMID: 35984314 Review.
-
Glycemic control and atrial fibrillation: an intricate relationship, yet under investigation.Cardiovasc Diabetol. 2022 Mar 14;21(1):39. doi: 10.1186/s12933-022-01473-0. Cardiovasc Diabetol. 2022. PMID: 35287684 Free PMC article. Review.
Cited by
-
Synergistic Effects of Weight Loss and Catheter Ablation: Can microRNAs Serve as Predictive Biomarkers for the Prevention of Atrial Fibrillation Recurrence?Int J Mol Sci. 2024 Apr 25;25(9):4689. doi: 10.3390/ijms25094689. Int J Mol Sci. 2024. PMID: 38731908 Free PMC article. Review.
-
The emerging role of extracellular vesicle RNAs as mediators of cardiometabolic diseases: from pathophysiology to clinical applications.Curr Opin Physiol. 2024 Aug;40:100764. doi: 10.1016/j.cophys.2024.100764. Epub 2024 May 31. Curr Opin Physiol. 2024. PMID: 40060218 Free PMC article.
References
-
- Lippi G, Sanchis‐Gomar F, Cervellin G. Global epidemiology of atrial fibrillation: an increasing epidemic and public health challenge. Int J Stroke. 2021;16(2):217‐221. - PubMed
-
- Hindricks G, Potpara T, Dagres N, et al. 2020 ESC guidelines for the diagnosis and management of atrial fibrillation developed in collaboration with the european association for cardio‐thoracic surgery (EACTS): the task force for the diagnosis and management of atrial fibrillation of the European society of cardiology (ESC) developed with the special contribution of the european heart rhythm association (EHRA) of the ESC. Eur Heart J. 2020;42(5):373‐498. - PubMed
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

