The Prevalence of the Virulence Genes of Staphylococcus aureus in Sickle Cell Disease Patients at KSUMC, Riyadh, Saudi Arabia
- PMID: 37508317
- PMCID: PMC10416153
- DOI: 10.3390/antibiotics12071221
The Prevalence of the Virulence Genes of Staphylococcus aureus in Sickle Cell Disease Patients at KSUMC, Riyadh, Saudi Arabia
Abstract
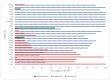
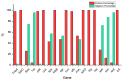
Staphylococcus aureus in the blood of sickle cell disease (SCD) patients may result in a significant increase in morbidity and mortality. S. aureus strains contain various virulence characteristics, including the ability to create a variety of toxins and develop drug resistance. The current study sought to assess the prevalence of S. aureus in SCD patients and to identify the pathogen's virulence characteristics. Between 2017 and 2021, blood samples and data were collected at King Saud University Medical City (KSUMC) in Riyadh, Saudi Arabia. The Vitek system PCR and gene sequencing methods were used for identification, antibiotic resistance patterns, and genetic analysis. During the study period, 47 S. aureus blood isolates (methicillin-resistant S. aureus (MRSA) 41.6% and non-MRSA 58.4%) were isolated from 2406 SCD patients. The prevalence percentages of virulence genes (finbB, sdrC, sdrD, icaA, coa, nuc, hlg, hla, finbA, clfA, efb, pvl, agr, spa, seb, sea, sec, tst, and sed) among all the isolates from the SCD patients compared with non-SCD patients (control group) were as follows: (100% vs. 100%), (100% vs. 100%), (100% vs. 100%), (100% vs. 87.5%), (100% vs. 81.3%), (100% vs. 100%), (100% vs. 100%), (100% vs. 100%), (97.9% vs. 81.3%), (97.9% vs. 100%), (97.9% vs. 87.5%), (54.3% vs. 56.3%), (46.8% vs. 75%), (42.6% vs. 43.8%), (27.7% vs. 0%), (25.5% vs. 12.5%), (12.8% vs. 6.3%), (4.3% vs. 12.5%), and (4.3% vs. 0%). Regarding the resistance genes (plaZ, mecA, ermA, ermC, tetK, tetM, and ermB) of the S. aureus strains isolated from the SCD patients compared with non-SCD patients (control group), the prevalence percentages were as follows: (100% vs. 100%), (100% vs. 56.3%), (0% vs. 31.3%), (31.9% vs. 18.8%), (40.4% vs. 25%), (0% vs. 0%), and (0% vs. 0%). As for the antibiotic (ampicillin, penicillin, amoxicillin, cefazolin, imipenem, oxacillin, erythromycin, tetracycline, azithromycin, ciprofloxacin, moxifloxacin, and levofloxacin) resistance of the S. aureus strains isolated from the SCD patients compared with non-SCD patients (control group), the prevalence percentages were as follows: (100% vs. 100%), (97.9% vs. 100%), (72.3% vs. 25%), (68.1% vs. 37.5%), (68.1% vs. 25%), (66% vs. 25%), (36.2% vs. 18.8%), (23.4% vs. 12.5%), (19.1% vs. 12.5%), (17% vs. 12.5%), (14.9% vs. 25%), and (10.6% vs. 18.7%). This study concluded that several virulence genes were present in the S. aureus strains recovered from the SCD patients at KSUMC, with all the isolates containing the finbB, sdrC, sdrD, icaA, coa, nuc, hlg, and hla genes.
Keywords: MRSA; Saudi Arabia; antibiotics; antimicrobial resistance; sickle cell disease; virulence factors.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
References
-
- Garoy E.Y., Gebreab Y.B., Achila O.O., Tekeste D.G., Kesete R., Ghirmay R., Kiflay R., Tesfu T. Methicillin-resistant Staphylococcus aureus (MRSA): Prevalence and antimicrobial sensitivity pattern among patients—A multicenter study in Asmara, Eritrea. Can. J. Infect. Dis. Med. Microbiol. 2019;2019:8321834. doi: 10.1155/2019/8321834. - DOI - PMC - PubMed
-
- Appiah V.A., Pesewu G.A., Kotey F.C., Boakye A.N., Duodu S., Tette E.M., Nyarko M.Y., Donkor E.S. Staphylococcus aureus nasal colonization among children with sickle cell disease at the Children’s Hospital, Accra: Prevalence, risk factors, and antibiotic resistance. Pathogens. 2020;9:329. doi: 10.3390/pathogens9050329. - DOI - PMC - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

