Fatigue Potentially Reduces the Effect of Transcranial Magnetic Stimulation on Depression Following COVID-19 and Its Vaccination
- PMID: 37514967
- PMCID: PMC10383898
- DOI: 10.3390/vaccines11071151
Fatigue Potentially Reduces the Effect of Transcranial Magnetic Stimulation on Depression Following COVID-19 and Its Vaccination
Abstract
COVID-19's long-term effects, known as Long-COVID, present psychiatric and physical challenges in recovered patients. Similarly, rare long-term post-vaccination side effects, resembling Long-COVID, are emerging (called Post-Vaccine). However, effective treatments for both conditions are scarce. Our clinical experience suggests that transcranial magnetic stimulation (TMS) often aids recovery in Long-COVID and Post-Vaccine patients. However, its effectiveness is reduced in patients with severe fatigue. Therefore, we retrospectively analysed Tokyo TMS Clinic's outpatient records (60 in total; mean age, 38 years) to compare Long-COVID and post-vaccine patients' characteristics and symptoms, assess the impact of TMS on their symptoms, and investigate the role of fatigue in depression recovery with TMS. The primary outcome was the regression coefficient of the initial fatigue score on depression score improvement using TMS. Secondary outcomes included psychiatric/physical scores before and after TMS and their improvement rates. We found no differences in the initial symptoms and background factors between Long-COVID and Post-Vaccine patients. After ten TMS sessions, all psychiatric and physical symptom scores improved significantly. TMS improves depression, insomnia, anxiety, and related neuropsychiatric symptoms, which were the primary complaints in this study. Thus, we conclude that TMS improves depression and anxiety. The effectiveness of TMS in treating depression in Long-COVID and Post-Vaccine patients decreased as fatigue severity increased. In conclusion, TMS relieved depressive symptoms following COVID-19 and vaccination; however, fatigue may hinder its effectiveness.
Keywords: fatigue; long-COVID; transcranial magnetic stimulation.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
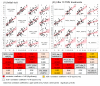


References
-
- Thompson E.J., Stafford J., Moltrecht B., Huggins C.F., Kwong A.S., Shaw R.J., Zaninotto P., Patel K., Silverwood R.J., McElroy E. Psychological distress, depression, anxiety, and life satisfaction following COVID-19 infection: Evidence from 11 UK longitudinal population studies. Lancet Psychiatry. 2022;9:894–906. doi: 10.1016/S2215-0366(22)00307-8. - DOI - PMC - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources

