A repeated cross-sectional analysis on the economic impact of SARS-CoV-2 pandemic at the hospital level in Italy
- PMID: 37524912
- PMCID: PMC10390582
- DOI: 10.1038/s41598-023-39592-7
A repeated cross-sectional analysis on the economic impact of SARS-CoV-2 pandemic at the hospital level in Italy
Erratum in
-
Author Correction: A repeated cross-sectional analysis on the economic impact of SARS-CoV-2 pandemic at the hospital level in Italy.Sci Rep. 2023 Sep 5;13(1):14610. doi: 10.1038/s41598-023-41716-y. Sci Rep. 2023. PMID: 37670133 Free PMC article. No abstract available.
Abstract
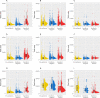
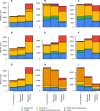
Italy was the first country in Europe to be hit by the Severe Acute Respiratory Syndrome Coronavirus 2. Little research has been conducted to understand the economic impact of providing care for SARS-CoV-2 patients during the pandemic. Our study aims to quantify the incremental healthcare costs for hospitalizations associated to being discharged before or after the first SARS-CoV-2 case was notified in Italy, and to a positive or negative SARS-CoV-2 notified infection. We used data on hospitalizations for 9 different diagnosis related groups at a large Italian Research Hospital with discharge date between 1st January, 2018 and 31st December 2021. The median overall costs for a hospitalization increased from 2410EUR (IQR: 1588-3828) before the start of the pandemic, to 2645EUR (IQR: 1885-4028) and 3834EUR (IQR: 2463-6413) during the pandemic, respectively for patients SARS-CoV-2 negative and positive patients. Interestingly, according to results of a generalized linear model, the highest increases in the average costs sustained for SARS-CoV-2 positive patients with respect to patients discharged before the pandemic was found among those with diagnoses unrelated to COVID-19, i.e. kidney and urinary tract infections with CC (59.71%), intracranial hemorrhage or cerebral infarction (53.33), and pulmonary edema and respiratory failure (47.47%). Our study highlights the economic burden during the COVID-19 pandemic on the hospital system in Italy based on individual patient data. These results contribute to the to the debate around the efficiency of the healthcare services provision during a pandemic.
© 2023. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures

References
-
- AGE.N.AS and ISTAT. Impatto dell’epidemia COVID-19 sul sistema ospedaliero italiano. Available at: https://www.agenas.gov.it/images/agenas/ISTAT/REPORT_IMPATTO_COVID_SU_RI.... Accessed 21 July 2022.
-
- De Filippo O, D'Ascenzo F, Angelini F, Bocchino PP, Conrotto F, Saglietto A, Secco GG, Campo G, Gallone G, Verardi R, Gaido L, Iannaccone M, Galvani M, Ugo F, Barbero U, Infantino V, Olivotti L, Mennuni M, Gili S, Infusino F, Vercellino M, Zucchetti O, Casella G, Giammaria M, Boccuzzi G, Tolomeo P, Doronzo B, Senatore G, Grosso Marra W, Rognoni A, Trabattoni D, Franchin L, Borin A, Bruno F, Galluzzo A, Gambino A, Nicolino A, Truffa Giachet A, Sardella G, Fedele F, Monticone S, Montefusco A, Omedè P, Pennone M, Patti G, Mancone M, De Ferrari GM. Reduced rate of hospital admissions for ACS during covid-19 outbreak in northern Italy. N. Engl. J. Med. 2020;383(1):88–89. doi: 10.1056/NEJMc2009166. - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

