Dynamic Trends and Underlying Factors of COVID-19 Vaccine Booster Hesitancy in Adults: Cross-Sectional Observational Study
- PMID: 37526963
- PMCID: PMC10395646
- DOI: 10.2196/44822
Dynamic Trends and Underlying Factors of COVID-19 Vaccine Booster Hesitancy in Adults: Cross-Sectional Observational Study
Abstract
Background: COVID-19 vaccine hesitancy reduces vaccination rates, which is detrimental to building herd immunity and halting the spread of COVID-19 and its variations. Most researches have simply identified the reasons affecting COVID-19 vaccination reluctance without delving into its dynamics, which makes forecasting future trends difficult.
Objective: This study aimed to examine the current COVID-19 vaccine booster hesitancy rate in Chinese adults as well as the dynamics of vaccine hesitancy and its influencing factors. The results of this study will have practical implications for policy responses in mainland China, and effective COVID-19 booster vaccination in specific populations.
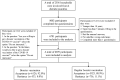
Methods: The web-based survey was completed by creating questionnaires and using a stratified random sampling method to collect information from adults (≥18 years old) among 2556 households in 4 geographical regions of China. We collected sociodemographic information, health status, awareness of COVID-19 and its vaccine, self-perceptions, trust in medical staff and vaccine developers, and so on. The odds ratios and 95% CI for the statistical associations were estimated using logistic regression models.
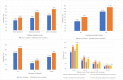
Results: Overall, 6659 participants (females: n=3540, 53.2%; males: n=3119, 46.8%) responded. In total, 533 (8%; 95% CI 7.4%-8.7%) participants presented a clear hesitancy in receiving the COVID-19 booster vaccination, while 736 (11.1%; 95% CI 10.3%-11.8%) expressed hesitancy in regular booster vaccination. A higher prevalence of vaccine hesitancy in both booster vaccination and regular booster vaccination was observed among participants with a history of allergies, experiencing chronic disease, lower levels of public health prevention measures or susceptibility or benefits or self-efficiency, higher levels of severity or barriers, and lower trust in both medical staff and vaccine developers (P<.05). The females and participants with higher education levels, higher levels of barriers, lower levels of susceptibility, and lower trust in vaccine developers preferred to have attitudinal changes from acceptance to hesitancy, while people with higher education levels, lower self-report health conditions, experiencing chronic disease, history of allergies, and lower trust in medical staff and developers were all positively associated with constant COVID-19 booster hesitancy.
Conclusions: The prevalence of COVID-19 vaccine booster hesitancy is not high in mainland China. However, there is a slight increment in hesitancy on regular booster vaccination. Conducting targeted information guidance for people with higher education levels and chronic diseases, as well as improving accessibility to booster vaccination and increasing trust in medical staff and vaccine producers may be highly effective in reducing vaccine hesitancy.
Keywords: COVID-19 booster vaccination; COVID-19 vaccine; China; influencing factors; vaccine hesitancy.
©Jian Wu, Mingze Ma, Quanman Li, Xinghong Guo, Clifford Silver Tarimo, Shiyu Jia, Xue Zhou, Meiyun Wang, Jianqin Gu, Yudong Miao, Beizhu Ye. Originally published in JMIR Public Health and Surveillance (https://publichealth.jmir.org), 01.08.2023.
Conflict of interest statement
Conflicts of Interest: None declared.
Figures



References
-
- Wang Z, Muecksch F, Schaefer-Babajew D, Finkin S, Viant C, Gaebler C, Hoffmann HH, Barnes CO, Cipolla M, Ramos V, Oliveira TY, Cho A, Schmidt F, Da Silva J, Bednarski E, Aguado L, Yee J, Daga M, Turroja M, Millard KG, Jankovic M, Gazumyan A, Zhao Z, Rice CM, Bieniasz PD, Caskey M, Hatziioannou T, Nussenzweig MC. Naturally enhanced neutralizing breadth against SARS-CoV-2 one year after infection. Nature. 2021;595(7867):426–431. doi: 10.1038/s41586-021-03696-9. https://www.nature.com/articles/s41586-021-03696-9 10.1038/s41586-021-03696-9 - DOI - PMC - PubMed
-
- Burki TK. Herd immunity for COVID-19. Lancet Respir Med. 2021;9(2):135–136. doi: 10.1016/S2213-2600(20)30555-5. https://www.thelancet.com/journals/lanres/article/PIIS2213-2600(20)30555... S2213-2600(20)30555-5 - DOI - PMC - PubMed
-
- Arce JSS, Warren SS, Meriggi NF, Scacco A, McMurry N, Voors M, Syunyaev G, Malik AA, Aboutajdine S, Adeojo O, Anigo D, Armand A, Asad S, Atyera M, Augsburg B, Awasthi M, Ayesiga GE, Bancalari A, Nyqvist MB, Borisova E, Bosancianu CM, García MRC, Cheema A, Collins E, Cuccaro F, Farooqi AZ, Fatima T, Fracchia M, Soria MLG, Guariso A, Hasanain A, Jaramillo S, Kallon S, Kamwesigye A, Kharel A, Kreps S, Levine M, Littman R, Malik M, Manirabaruta G, Mfura JLH, Momoh F, Mucauque A, Mussa I, Nsabimana JA, Obara I, Otálora MJ, Ouédraogo BW, Pare TB, Platas MR, Polanco L, Qureshi JA, Raheem M, Ramakrishna V, Rendrá I, Shah T, Shaked SE, Shapiro JN, Svensson J, Tariq A, Tchibozo AM, Tiwana HA, Trivedi B, Vernot C, Vicente PC, Weissinger LB, Zafar B, Zhang B, Karlan D, Callen M, Teachout M, Humphreys M, Mobarak AM, Omer SB. COVID-19 vaccine acceptance and hesitancy in low- and middle-income countries. Nat Med. 2021;27(8):1385–1394. doi: 10.1038/s41591-021-01454-y. https://www.nature.com/articles/s41591-021-01454-y 10.1038/s41591-021-01454-y - DOI - PMC - PubMed
-
- Adams K, Rhoads JP, Surie D, Gaglani M, Ginde AA, McNeal T, Talbot HK, Casey JD, Zepeski A, Shapiro NI, Gibbs KW, Files DC, Hager DN, Frosch AE, Exline MC, Mohamed A, Johnson NJ, Steingrub JS, Peltan ID, Brown SM, Martin ET, Lauring AS, Khan A, Busse LW, Duggal A, Wilson JG, Chang SY, Mallow C, Kwon JH, Chappell JD, Halasa N, Grijalva CG, Lindsell CJ, Lester SN, Thornburg NJ, Park S, McMorrow ML, Patel MM, Tenforde MW, Self WH, Influenza and other Viruses in the AcutelY ill (IVY) Network Vaccine effectiveness of primary series and booster doses against covid-19 associated hospital admissions in the United States: living test negative design study. BMJ. 2022;379:e072065. doi: 10.1136/bmj-2022-072065. https://www.bmj.com/content/379/bmj-2022-072065 - DOI - PMC - PubMed
-
- Gupta PS, Mohareb AM, Valdes C, Price C, Jollife M, Regis C, Munshi N, Taborda E, Lautenschlager M, Fox A, Hanscom D, Kruse G, LaRocque R, Betancourt J, Taveras EM. Mobile health services for COVID-19: counseling, testing, and vaccination for medically underserved populations. Am J Public Health. 2022;112(11):1556–1559. doi: 10.2105/AJPH.2022.307021. https://ajph.aphapublications.org/doi/full/10.2105/AJPH.2022.307021 - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
Supplementary concepts
LinkOut - more resources
Full Text Sources
Medical

