A Prediction Model for Severe Maternal Morbidity and Mortality After Delivery Hospitalization
- PMID: 37535951
- PMCID: PMC10526683
- DOI: 10.1097/AOG.0000000000005281
A Prediction Model for Severe Maternal Morbidity and Mortality After Delivery Hospitalization
Abstract
Objective: To develop a risk stratification model for severe maternal morbidity (SMM) or mortality after the delivery hospitalization based on information available at the time of hospital discharge.
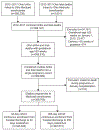
Methods: This population-based cohort study included all pregnancies among Ohio residents with Medicaid insurance from 2012 to 2017. Pregnant individuals were identified using linked live birth and fetal death records and Medicaid claims data. Inclusion was restricted to those with continuous postpartum Medicaid enrollment and delivery at 20 or more weeks of gestation. The primary outcome of the study was SMM or mortality after the delivery hospitalization and was assessed up to 42 days postpartum and up to 1 year postpartum separately. Variables considered for the model included patient-, obstetric health care professional-, and system-level data available in vital records or Medicaid claims data. Parsimonious models were created with logistic regression and were internally validated. Receiver operating characteristic curves were used to evaluate model performance, and model calibration was assessed.
Results: There were 343,842 pregnant individuals who met inclusion criteria with continuous Medicaid enrollment through 42 days postpartum and 287,513 with continuous enrollment through 1 year. After delivery hospitalization discharge, the incidence of SMM or mortality was 140.5 per 10,000 pregnancies through 42 days of delivery and 330.7 per 10,000 pregnancies through 1 year postpartum. The final model predicting SMM or mortality through 42 days postpartum included maternal prepregnancy body mass index, age, gestational age at delivery, mode of delivery, chorioamnionitis, and maternal diagnosis of cardiac disease, preeclampsia or gestational hypertension, or a mental health condition. Similar variables were included in the model predicting SMM or mortality through 365 days with chronic hypertension, pregestational diabetes, and illicit substance use added and chorioamnionitis removed. Both models demonstrated moderate prediction (area under the curve [AUC] 0.77, 95% CI 0.76-0.78 for 42-day model; AUC 0.72, 95% CI 0.71-0.73 for the 1-year model) and good calibration.
Conclusion: A prediction model for SMM or mortality up to 1 year postpartum was created and internally validated with information available to health care professionals at the time of hospital discharge. The utility of this model for patient counseling and strategies to optimize postpartum care for high-risk individuals will require further evaluation.
Copyright © 2023 by the American College of Obstetricians and Gynecologists. Published by Wolters Kluwer Health, Inc. All rights reserved.
Conflict of interest statement
Financial Disclosure The authors did not report any potential conflicts of interest.
Figures

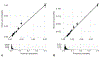
References
-
- Trost S, Beauregard J, Chandra G, Njie F, et al. Pregnancy-related deaths: data from maternal mortality review committees in 36 US States, 2017-2019. Atlanta, GA: Centers for Disease Control and Prevention, US Department of Helath and Human Services; 2022.
-
- Callaghan WM, Creanga AA, Kuklina EV. Severe maternal morbidity among delivery and postpartum hospitalizations in the United States. Obstet Gynecol. 2012;120(5):1029–1036. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous

