Trends in laboratory-confirmed bacterial meningitis (2012-2019): national observational study, England
- PMID: 37538400
- PMCID: PMC10393823
- DOI: 10.1016/j.lanepe.2023.100692
Trends in laboratory-confirmed bacterial meningitis (2012-2019): national observational study, England
Abstract
Background: Bacterial meningitis is associated with significant morbidity and mortality worldwide. We aimed to describe the epidemiology, aetiology, trends over time and outcomes of laboratory-confirmed bacterial meningitis in England during 2012-2019.
Methods: UK Health Security Agency routinely receives electronic notifications of confirmed infections from National Health Service hospital laboratories in England. Data were extracted for positive bacterial cultures, PCR-positive results for Neisseria meningitidis or Streptococcus pneumoniae from cerebrospinal fluid and positive blood cultures in patients with clinical meningitis.
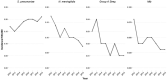
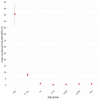
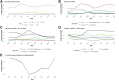
Findings: During 2012-19, there were 6554 laboratory-confirmed cases. Mean annual incidence was 1.49/100,000, which remained stable throughout the surveillance period (p = 0.745). There were 155 different bacterial species identified, including 68.4% (106/1550) Gram-negative and 31.6% (49/155) Gram-positive bacteria. After excluding coagulase-negative staphylococci (2481/6554, 37.9%), the main pathogens causing meningitis were Streptococcus pneumoniae (811/4073, 19.9%), Neisseria meningitidis (497/4073, 12.2%), Staphylococcus aureus (467/4073, 11.5%), Escherichia coli (314/4073, 7.7%) and group B streptococcus (268/4073, 6.6%). Pneumococcal meningitis incidence increased significantly during 2012-9, while meningococcal, group A streptococcal and tuberculous meningitis declined. Infants aged <3 months had the highest mean incidence (55.6/100,000; 95% CI, 47.7-63.5) driven mainly by group B streptococci, followed by 3-11 month-olds (8.1/100,000; 95% CI 7.1-9.0), where pneumococcal and meningitis predominated. The 30-day case-fatality rate (CFR) was 10.0% (71/6554). Group A streptococcal meningitis had the highest CFR (47/85, 55.3%). The probability of surviving at 30 days was 95.3% (95% CI, 93.4-97.3%) for infants and 80.0% for older adults (77-84%).
Interpretation: The incidence of bacterial meningitis has remained stable. The high CFR highlights a need for prevention through vaccination.
Funding: PHE.
Keywords: Bacterial meningitis; Group B streptococci; Meningococcal meningitis; Pneumococcal meningitis; Surveillance.
Crown Copyright © 2023 Published by Elsevier Ltd.
Conflict of interest statement
The authors declare no conflicts of interest.
Figures
References
-
- Excellence, NICE: National Institute for Health and Care . 2020. Meningitis - bacterial meningitis and meningococcal disease.https://cks.nice.org.uk/topics/meningitis-bacterial-meningitis-meningoco... [cited 2021 Jun 22]. Available from:
-
- Edmond K., Clark A., Korczak V.S., Sanderson C., Griffiths U.K., Rudan I. Global and regional risk of disabling sequelae from bacterial meningitis: a systematic review and meta-analysis. Lancet Infect Dis. 2010;10(5):317–328. - PubMed
-
- England, Public Health . 2013. Haemophilus influenzae: guidance, data and analysis.https://www.gov.uk/government/collections/haemophilus-influenzae-guidanc... Available from:
-
- Ladhani S.N., Andrews N., Parikh S.R., et al. Vaccination of infants with meningococcal group B vaccine (4CMenB) in England. N Engl J Med. 2020;382(4):309–317. - PubMed
LinkOut - more resources
Full Text Sources

