Lysophospholipids Are Associated With Outcomes in Hospitalized Patients With Mild Traumatic Brain Injury
- PMID: 37551969
- PMCID: PMC11071087
- DOI: 10.1089/neu.2023.0046
Lysophospholipids Are Associated With Outcomes in Hospitalized Patients With Mild Traumatic Brain Injury
Abstract
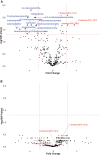
Mild traumatic brain injury (mTBI) accounts for 70-90% of all TBI cases. Lipid metabolites have important roles in plasma membrane biogenesis, function, and cell signaling. As TBI can compromise plasma membrane integrity and alter brain cell function, we sought to identify circulating phospholipid alterations after mTBI, and determine if these changes were associated with clinical outcomes. Patients with mTBI (Glasgow Coma Score [GCS] ≥13 and loss of consciousness <30 min) were recruited. A total of 84 mTBI subjects were enrolled after admission to a level I trauma center, with the majority having evidence of traumatic intracranial hemorrhage on brain computed tomography (CT). Plasma samples were collected within 24 h of injury with 32 mTBI subjects returning at 3 months after injury for a second plasma sample to be collected. Thirty-five healthy volunteers were enrolled as controls and had a one-time blood draw. Lipid metabolomics was performed on plasma samples from each subject. Fold change of selected lipid metabolites was determined. Multivariable regression models were created to test associations between lipid metabolites and discharge and 6-month Glasgow Outcomes Scale-Extended (GOSE) outcomes (dichotomized between "good" [GOSE ≥7] and "bad" [GOSE ≤6] functional outcomes). Plasma levels of 31 lipid metabolites were significantly associated with discharge GOSE using univariate models; three of these metabolites were significantly increased, while 14 were significantly decreased in subjects with good outcomes compared with subjects with poor outcomes. In multivariable logistic regression models, higher circulating levels of the lysophospholipids (LPL) 1-linoleoyl-glycerophosphocholine (GPC) (18:2), 1-linoleoyl-GPE (18:2), and 1-linolenoyl-GPC (18:3) were associated with both good discharge GOSE (odds ratio [OR] 12.2 [95% CI 3.35, 58.3], p = 5.23 × 10-4; OR 9.43 [95% CI 2.87, 39.6], p = 7.26 × 10-4; and OR 5.26 [95% CI 1.99, 16.7], p = 2.04 × 10-3, respectively) and 6-month (OR 4.67 [95% CI 1.49, 17.7], p = 0.013; OR 2.93 [95% CI 1.11, 8.87], p = 0.039; and OR 2.57 [95% CI 1.08, 7.11], p = 0.046, respectively). Compared with healthy volunteers, circulating levels of these three LPLs were decreased early after injury and had normalized by 3 months after injury. Logistic regression models to predict functional outcomes were created by adding each of the described three LPLs to a baseline model that included age and sex. Including 1-linoleoyl-GPC (18:2) (8.20% improvement, p = 0.009), 1-linoleoyl-GPE (18:2) (8.85% improvement, p = 0.021), or 1-linolenoyl-GPC (18:3) (7.68% improvement, p = 0.012), significantly improved the area under the curve (AUC) for predicting discharge outcomes compared with the baseline model. Models including 1-linoleoyl-GPC (18:2) significantly improved AUC for predicting 6-month outcomes (9.35% improvement, p = 0.034). Models including principal components derived from 25 LPLs significantly improved AUC for prediction of 6-month outcomes (16.0% improvement, p = 0.020). Our results demonstrate that higher plasma levels of LPLs (1-linoleoyl-GPC, 1-linoleoyl-GPE, and 1-linolenoyl-GPC) after mTBI are associated with better functional outcomes at discharge and 6 months after injury. This class of phospholipids may represent a potential therapeutic target.
Keywords: biomarkers; lysophospholipids; mild traumatic brain injury; outcomes.
Conflict of interest statement
No competing financial interests exist.
Figures




Similar articles
-
Pathological Computed Tomography Features Associated With Adverse Outcomes After Mild Traumatic Brain Injury: A TRACK-TBI Study With External Validation in CENTER-TBI.JAMA Neurol. 2021 Sep 1;78(9):1137-1148. doi: 10.1001/jamaneurol.2021.2120. JAMA Neurol. 2021. PMID: 34279565 Free PMC article.
-
Prognostic Models for Global Functional Outcome and Post-Concussion Symptoms Following Mild Traumatic Brain Injury: A Collaborative European NeuroTrauma Effectiveness Research in Traumatic Brain Injury (CENTER-TBI) Study.J Neurotrauma. 2023 Aug;40(15-16):1651-1670. doi: 10.1089/neu.2022.0320. Epub 2023 May 24. J Neurotrauma. 2023. PMID: 37078144 Free PMC article.
-
Computed Tomography Lesions and Their Association With Global Outcome in Young People With Mild Traumatic Brain Injury.J Neurotrauma. 2023 Jun;40(11-12):1243-1254. doi: 10.1089/neu.2022.0055. Epub 2023 Feb 24. J Neurotrauma. 2023. PMID: 36578216
-
Animal Models for Concussion: Molecular and Cognitive Assessments—Relevance to Sport and Military Concussions.In: Kobeissy FH, editor. Brain Neurotrauma: Molecular, Neuropsychological, and Rehabilitation Aspects. Boca Raton (FL): CRC Press/Taylor & Francis; 2015. Chapter 46. In: Kobeissy FH, editor. Brain Neurotrauma: Molecular, Neuropsychological, and Rehabilitation Aspects. Boca Raton (FL): CRC Press/Taylor & Francis; 2015. Chapter 46. PMID: 26269898 Free Books & Documents. Review.
-
Prognostic Significance of Magnetic Resonance Imaging in Detecting Diffuse Axonal Injuries: Analysis of Outcomes and Review of Literature.Neurol India. 2022 Nov-Dec;70(6):2371-2377. doi: 10.4103/0028-3886.364066. Neurol India. 2022. PMID: 36537418 Review.
Cited by
-
Systemic Metabolic Alterations after Aneurysmal Subarachnoid Hemorrhage: A Plasma Metabolomics Approach.medRxiv [Preprint]. 2025 Jan 7:2025.01.06.25320083. doi: 10.1101/2025.01.06.25320083. medRxiv. 2025. PMID: 39830284 Free PMC article. Preprint.
-
Glycerophospholipid dysregulation after traumatic brain injury.Neurochem Int. 2024 May;175:105701. doi: 10.1016/j.neuint.2024.105701. Epub 2024 Feb 28. Neurochem Int. 2024. PMID: 38428503 Free PMC article. Review.
-
Plasma biomarkers for brain injury in extracorporeal membrane oxygenation.Acute Crit Care. 2023 Nov;38(4):389-398. doi: 10.4266/acc.2023.01368. Epub 2023 Nov 29. Acute Crit Care. 2023. PMID: 38052506 Free PMC article.
-
Metabolomic and lipidomic pathways in aneurysmal subarachnoid hemorrhage.Neurotherapeutics. 2025 Jan;22(1):e00504. doi: 10.1016/j.neurot.2024.e00504. Epub 2024 Dec 19. Neurotherapeutics. 2025. PMID: 39701893 Free PMC article. Review.
-
Exploring Lysophosphatidylcholine as a Biomarker in Ischemic Stroke: The Plasma-Brain Disjunction.Int J Mol Sci. 2024 Oct 3;25(19):10649. doi: 10.3390/ijms251910649. Int J Mol Sci. 2024. PMID: 39408978 Free PMC article.
References
-
- Center for Disease Control and Prevention. Report to Congress on Traumatic Brain Injury in the United States: Epidemiology and Rehabilitation. National Center for Injury Prevention and Control, Division of Unintentional Injury Prevention: Atlanta; 2015.
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials
