Bioadhesive polymer semiconductors and transistors for intimate biointerfaces
- PMID: 37561870
- PMCID: PMC10768720
- DOI: 10.1126/science.adg8758
Bioadhesive polymer semiconductors and transistors for intimate biointerfaces
Abstract
The use of bioelectronic devices relies on direct contact with soft biotissues. For transistor-type bioelectronic devices, the semiconductors that need to have direct interfacing with biotissues for effective signal transduction do not adhere well with wet tissues, thereby limiting the stability and conformability at the interface. We report a bioadhesive polymer semiconductor through a double-network structure formed by a bioadhesive brush polymer and a redox-active semiconducting polymer. The resulting semiconducting film can form rapid and strong adhesion with wet tissue surfaces together with high charge-carrier mobility of ~1 square centimeter per volt per second, high stretchability, and good biocompatibility. Further fabrication of a fully bioadhesive transistor sensor enabled us to produce high-quality and stable electrophysiological recordings on an isolated rat heart and in vivo rat muscles.
Conflict of interest statement
Figures


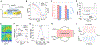


References
-
- Sunwoo S-H, Ha K-H, Lee S, Lu N, Kim D-H, Wearable and Implantable Soft Bioelectronics: Device Designs and Material Strategies. Annual Review of Chemical and Biomolecular Engineering 12, 359–391 (2021). - PubMed
-
- Yuk H, Lu B, Zhao X, Hydrogel bioelectronics. Chem Soc Rev 48, 1642–1667 (2019). - PubMed
-
- You I et al. , Artificial multimodal receptors based on ion relaxation dynamics. Science 370, 961–965 (2020). - PubMed
-
- Liu S, Rao Y, Jang H, Tan P, Lu N, Strategies for body-conformable electronics. Matter 5, 1104–1136 (2022).
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

