Carbon Monoxide Poisoning: From Microbes to Therapeutics
- PMID: 37582490
- PMCID: PMC11160397
- DOI: 10.1146/annurev-med-052422-020045
Carbon Monoxide Poisoning: From Microbes to Therapeutics
Abstract
Carbon monoxide (CO) poisoning leads to 50,000-100,000 emergency room visits and 1,500-2,000 deaths each year in the United States alone. Even with treatment, survivors often suffer from long-term cardiac and neurocognitive deficits, highlighting a clear unmet medical need for novel therapeutic strategies that reduce morbidity and mortality associated with CO poisoning. This review examines the prevalence and impact of CO poisoning and pathophysiology in humans and highlights recent advances in therapeutic strategies that accelerate CO clearance and mitigate toxicity. We focus on recent developments of high-affinity molecules that take advantage of the uniquely strong interaction between CO and heme to selectively bind and sequester CO in preclinical models. These scavengers, which employ heme-binding scaffolds ranging from organic small molecules to hemoproteins derived from humans and potentially even microorganisms, show promise as field-deployable antidotes that may rapidly accelerate CO clearance and improve outcomes for survivors of acute CO poisoning.
Keywords: antidotes; carbon monoxide; carbon monoxide poisoning; heme; mitochondria.
Figures

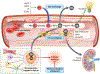
References
-
- Motterlini R, Otterbein LE. 2010. The therapeutic potential of carbon monoxide. Nat. Rev. Drug Discov. 9:728–43 - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

