Effect of gender on the association between cumulative cardiovascular risk factors and depression: results from the US National Health and Nutrition Examination Survey
- PMID: 37600975
- PMCID: PMC10432622
- DOI: 10.1136/gpsych-2023-101063
Effect of gender on the association between cumulative cardiovascular risk factors and depression: results from the US National Health and Nutrition Examination Survey
Abstract
Background: The comorbidity of cardiovascular disease (CVD) and depression has been well established, as depression usually presents simultaneously with CVD risk factors. However, the potential association between cumulative exposure to CVD risk and depression remains unclear, so we conducted the current investigation. To our knowledge, this is the first study that employs the cumulative risk model to examine the effect of CVD risk factors on depression using nationally representative population and gender, age and CVD status-stratified subpopulations.
Aims: To systematically study the possible individual and cumulative effect of 18 CVD risk factors on depression.
Methods: A cross-sectional, secondary analysis investigated associations between 18 CVD risk factors and depression. The interaction effect between CVD risk factors and age, gender and CVD status was also examined. Enrolment included 20 816 participants from the US National Health and Nutrition Examination Survey 2005-2016. Participants with Patient Health Questionnaire-9 scores over 15 or who were using an antidepressant were considered depressive; 18 known cardiovascular risk factors were incorporated in the present study.
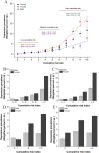
Results: At the individual risk factor level, smoking, drinking, living alone, sleep quality, body mass index, waist circumference and diabetes status had differential associations with depression risk according to the gender, age or CVD status of the participants. Most importantly, gender-stratified cumulative risk analysis indicated that similar depression risk was found in both genders with a small number of CVD risk factors (odds ratio (OR)adjusted=1.32; 95% confidence interval (CI): 0.87 to 1.99), but females had a significantly higher depression risk compared with males under high cumulative risk exposure (ORadjusted=2.86; 95% CI: 1.79 to 4.59).
Conclusions: Clarifying the association of numerous CVD risk factors with depression according to gender, age and overall CVD status may be beneficial for risk stratification and the prevention of depression in clinical practice. Moreover, the observed novel evidence of high cumulative risk exposure-mediated gender disparities in depression risk may shed light on the underlying mechanism of females' greater vulnerability to depression.
Keywords: Depression.
© Author(s) (or their employer(s)) 2023. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ.
Conflict of interest statement
Competing interests: None declared.
Figures

Similar articles
-
Association between depression and cardiovascular disease risk in general population of Korea: results from the Korea National Health and Nutrition Examination Survey, 2016.Ann Occup Environ Med. 2019 Jun 20;31:e10. doi: 10.35371/aoem.2019.31.e10. eCollection 2019. Ann Occup Environ Med. 2019. PMID: 31543971 Free PMC article.
-
The role of traditional risk factors in explaining the social disparities in cardiovascular death: The national health and Nutrition Examination Survey III (NHANES III).Am J Prev Cardiol. 2020 Oct 15;4:100094. doi: 10.1016/j.ajpc.2020.100094. eCollection 2020 Dec. Am J Prev Cardiol. 2020. PMID: 34327470 Free PMC article.
-
Sleep disordered breathing may not be an independent risk factor for diabetes, but diabetes may contribute to the occurrence of periodic breathing in sleep.Sleep Med. 2003 Jul;4(4):349-50. doi: 10.1016/s1389-9457(03)00118-7. Sleep Med. 2003. PMID: 14592310
-
Risk of Cardiovascular Disease Mortality in Relation to Depression and 14 Common Risk Factors.Int J Gen Med. 2021 Feb 12;14:441-449. doi: 10.2147/IJGM.S292140. eCollection 2021. Int J Gen Med. 2021. PMID: 33603451 Free PMC article.
-
Association of sleep-related disorders with cardiovascular disease among adults in the United States: A cross-sectional study based on national health and nutrition examination survey 2005-2008.Front Cardiovasc Med. 2022 Aug 4;9:954238. doi: 10.3389/fcvm.2022.954238. eCollection 2022. Front Cardiovasc Med. 2022. PMID: 35990939 Free PMC article.
Cited by
-
Bidirectional associations between mental disorders, antidepressants and cardiovascular disease.BMJ Ment Health. 2024 Mar 15;27(1):e300975. doi: 10.1136/bmjment-2023-300975. BMJ Ment Health. 2024. PMID: 38490691 Free PMC article.
-
The mediating role of sleep disturbance in the relationship between depression and cardiovascular disease.Front Psychiatry. 2024 Jun 5;15:1417179. doi: 10.3389/fpsyt.2024.1417179. eCollection 2024. Front Psychiatry. 2024. PMID: 38903636 Free PMC article.
-
Causal relationship between depression and hypercholesterolemia: A bidirectional 2-sample Mendelian randomization study.Medicine (Baltimore). 2024 May 24;103(21):e38234. doi: 10.1097/MD.0000000000038234. Medicine (Baltimore). 2024. PMID: 38788001 Free PMC article.
-
Psychological interventions for post-stroke anxiety and depression: Current approaches and future perspectives.World J Psychiatry. 2025 Jun 19;15(6):103270. doi: 10.5498/wjp.v15.i6.103270. eCollection 2025 Jun 19. World J Psychiatry. 2025. PMID: 40574760 Free PMC article. Review.
-
Association between plant-based diets and depression in older adults with heart disease: the mediating role of sleep disturbances.Front Nutr. 2025 Apr 16;12:1567436. doi: 10.3389/fnut.2025.1567436. eCollection 2025. Front Nutr. 2025. PMID: 40308641 Free PMC article.
References
LinkOut - more resources
Full Text Sources
