Prophylactic Lymphovenous Bypass at the Time of Axillary Lymph Node Dissection Decreases Rates of Lymphedema
- PMID: 37601478
- PMCID: PMC10431289
- DOI: 10.1097/AS9.0000000000000278
Prophylactic Lymphovenous Bypass at the Time of Axillary Lymph Node Dissection Decreases Rates of Lymphedema
Abstract
Background: Breast cancer-related lymphedema impacts 30% to 47% of women who undergo axillary lymph node dissection (ALND). Studies evaluating the effectiveness of prophylactic lymphovenous bypass (LVB) at the time of ALND have had small patient populations and/or short follow-up. The aim of this study is to quantitatively and qualitatively evaluate prophylactic LVB in patients with breast cancer.
Methods: A retrospective review of patients who underwent ALND from 2018 to 2022 was performed. Patients were divided into cohorts based on whether they underwent prophylactic LVB at the time of ALND. Primary outcomes included 30-day complications and lymphedema. Lymphedema was quantitatively evaluated by bioimpedance analysis, with L-dex scores >7.1 indicating lymphedema.
Results: One-hundred five patients were identified. Sixty-four patients (61.0%) underwent ALND and 41 patients (39.0%) underwent ALND+LVB. Postoperative complications were similar between the cohorts. At a median follow-up of 13.3 months, lymphedema occurred significantly higher in the ALND only group compared with ALND+LVB group (50.0% vs 12.2%; P < 0.001). ALND without LVB was an independent risk factor for lymphedema development (odds ratio, 4.82; P = 0.003).
Conclusions: Prophylactic LVB decreases lymphedema and is not associated with increased postoperative complications. A multidisciplinary team approach is imperative to decrease lymphedema development in this patient population.
Keywords: lyMPHA; lymphedema; lymphovenous bypass; microsurgery; super-microsurgery.
Copyright © 2023 The Author(s). Published by Wolters Kluwer Health, Inc.
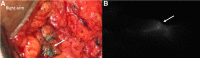
Figures

Similar articles
-
Preventing Breast Cancer-Related Lymphedema: A Comprehensive Analysis of a 9-Year Single-Center Experience of Prophylactic Lymphovenous Bypass.Ann Surg Oncol. 2025 Mar;32(3):2007-2015. doi: 10.1245/s10434-024-16640-8. Epub 2024 Dec 23. Ann Surg Oncol. 2025. PMID: 39715967
-
National Outcomes of Prophylactic Lymphovenous Bypass during Axillary Lymph Node Dissection.J Reconstr Microsurg. 2022 Oct;38(8):613-620. doi: 10.1055/s-0042-1742730. Epub 2022 Feb 14. J Reconstr Microsurg. 2022. PMID: 35158396
-
Lymphovenous Coupler-Assisted Bypass for Immediate Lymphatic Reconstruction.J Reconstr Microsurg. 2024 Jun;40(5):334-347. doi: 10.1055/a-2181-7559. Epub 2023 Sep 26. J Reconstr Microsurg. 2024. PMID: 37751886
-
Is bioimpedance spectroscopy a useful tool for objectively assessing lymphovenous bypass surgical outcomes in breast cancer-related lymphedema?Breast Cancer Res Treat. 2021 Feb;186(1):1-6. doi: 10.1007/s10549-020-06059-6. Epub 2021 Jan 4. Breast Cancer Res Treat. 2021. PMID: 33392840 Review.
-
Lymphedema Incidence After Axillary Lymph Node Dissection: Quantifying the Impact of Radiation and the Lymphatic Microsurgical Preventive Healing Approach.Ann Plast Surg. 2019 Apr;82(4S Suppl 3):S234-S241. doi: 10.1097/SAP.0000000000001864. Ann Plast Surg. 2019. PMID: 30855393 Review.
Cited by
-
Racial Disparities in Breast Cancer: from Detection to Treatment.Curr Oncol Rep. 2024 Jan;26(1):10-20. doi: 10.1007/s11912-023-01472-8. Epub 2023 Dec 15. Curr Oncol Rep. 2024. PMID: 38100011 Review.
-
Immediate lymphatic reconstruction for breast cancer-related lymphedema prevention: A systematic review.JPRAS Open. 2025 Apr 4;44:448-462. doi: 10.1016/j.jpra.2025.03.021. eCollection 2025 Jun. JPRAS Open. 2025. PMID: 40452891 Free PMC article.
-
Axillary Surgical Management in Breast Cancer Patients after Neoadjuvant Systemic Therapy: A Delphi Study.Breast Care (Basel). 2025 May 10:1-9. doi: 10.1159/000546267. Online ahead of print. Breast Care (Basel). 2025. PMID: 40584028 Free PMC article.
-
Preventing Breast Cancer-Related Lymphedema: A Comprehensive Analysis of a 9-Year Single-Center Experience of Prophylactic Lymphovenous Bypass.Ann Surg Oncol. 2025 Mar;32(3):2007-2015. doi: 10.1245/s10434-024-16640-8. Epub 2024 Dec 23. Ann Surg Oncol. 2025. PMID: 39715967
References
-
- Fu MR, Kang Y. Psychosocial impact of living with cancer-related lymphedema. Semin Oncol Nurs. 2013;29:50–60. - PubMed
-
- Grada AA, Phillips TJ. Lymphedema: pathophysiology and clinical manifestations. J Am Acad Dermatol. 2017;77:1009–1020. - PubMed
-
- Lee JH, Chang DW. Surgical treatment of primary lymphedema. Lymphat Res Biol. 2017;15:220–226. - PubMed
-
- Morrell RM, Halyard MY, Schild SE, et al. . Breast cancer-related lymphedema. Mayo Clin Proc. 2005;80:1480–1484. - PubMed
LinkOut - more resources
Full Text Sources

