This is a preprint.
Material Properties of Nonpregnant and Pregnant Human Uterine Layers
- PMID: 37609213
- PMCID: PMC10441310
- DOI: 10.1101/2023.08.07.551726
Material Properties of Nonpregnant and Pregnant Human Uterine Layers
Update in
-
Material properties of nonpregnant and pregnant human uterine layers.J Mech Behav Biomed Mater. 2024 Mar;151:106348. doi: 10.1016/j.jmbbm.2023.106348. Epub 2023 Dec 28. J Mech Behav Biomed Mater. 2024. PMID: 38198930 Free PMC article.
Abstract
The uterus has critical biomechanical functions in pregnancy and undergoes dramatic material growth and remodeling from implantation to parturition. The intrinsic material properties of the human uterus and how they evolve in pregnancy are poorly understood. To address this knowledge gap and assess the heterogeneity of these tissues, the time-dependent material properties of all human uterine layers were measured with nanoindentation. The endometrium-decidua layer was found to be the least stiff, most viscous, and least permeable layer of the human uterus in nonpregnant and third-trimester pregnant tissues. In pregnancy, endometrium-decidua becomes stiffer and less viscous with no material property changes observed in the myometrium or perimetrium. Additionally, uterine material properties did not significantly differ between third-trimester pregnant tissues with and without placenta accreta. The foundational data generated by this study will facilitate the development of physiologically accurate models of the human uterus to investigate gynecologic and obstetric disorders.
Keywords: Reproductive biomechanics; nanoindentation; poro-viscoelasticity; pregnancy; uterus.
Figures



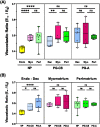

References
-
- 2019 Assisted Reproductive Technology Fertility Clinic and National Summary Report. Published online 2019:112.
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources
Miscellaneous
