Emergent conversion from single-anastomosis gastric bypass to Roux-en-Y gastric bypass with subsequent obstruction of entero-enteric anastomosis by ascaris
- PMID: 37614466
- PMCID: PMC10444309
- DOI: 10.1093/jscr/rjad428
Emergent conversion from single-anastomosis gastric bypass to Roux-en-Y gastric bypass with subsequent obstruction of entero-enteric anastomosis by ascaris
Abstract
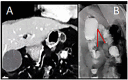
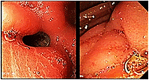
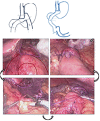
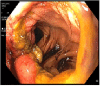
One anastomosis gastric bypass (OAGB), the third most commonly performed procedure worldwide, has shown excellent results in terms of weight loss and resolution of comorbidities compared with other bariatric surgeries. However, its use remains limited in various parts of the world due to postoperative complications. After the efficacy of this procedure was established, the focus of treatment shifted toward resolving postoperative complications. Protein-energy malnutrition after OAGB is one of the main issues that needs to be addressed. There are several operative options for patients who require revision surgery including reversal and conversion to Roux-en-Y gastric bypass (RYGB). The conversion from OAGB to RYGB is a feasible method that has shown excellent results when performed by experts in the field. Here, we present the case of a woman with symptoms of acute obstruction secondary to OAGB who underwent conversion to RYGB under emergent conditions.
Keywords: OAGB; RYGB; bariatric surgery; complications; obstruction.
Published by Oxford University Press and JSCR Publishing Ltd. © The Author(s) 2023.
Conflict of interest statement
None declared.
Figures
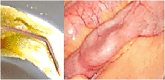
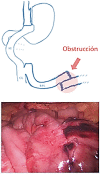
Similar articles
-
Conversion from one-anastomosis gastric bypass to Roux-en-Y gastric bypass: when and why-a single-center experience of all consecutive OAGB procedures.Surg Obes Relat Dis. 2022 Feb;18(2):225-232. doi: 10.1016/j.soard.2021.10.019. Epub 2021 Oct 27. Surg Obes Relat Dis. 2022. PMID: 34794865
-
Conversion of One Anastomosis Gastric Bypass (OAGB) to Roux-en-Y Gastric Bypass (RYGB) for Biliary Reflux Resistant to Medical Treatment: Lessons Learned from a Retrospective Series of 2780 Consecutive Patients Undergoing OAGB.Obes Surg. 2020 Jun;30(6):2093-2098. doi: 10.1007/s11695-020-04460-0. Obes Surg. 2020. PMID: 32052289
-
Conversion of One Anastomosis Gastric Bypass to Roux-en-Y Gastric Bypass: Results of a Retrospective Multicenter Study.Obes Surg. 2022 Jun;32(6):1842-1848. doi: 10.1007/s11695-022-05963-8. Epub 2022 Feb 25. Obes Surg. 2022. PMID: 35212908
-
Randomized Controlled Trial of One Anastomosis Gastric Bypass Versus Roux-En-Y Gastric Bypass for Obesity: Comparison of the YOMEGA and Taiwan Studies.Obes Surg. 2019 Sep;29(9):3047-3053. doi: 10.1007/s11695-019-04065-2. Obes Surg. 2019. PMID: 31290104 Review.
-
One Anastomosis Gastric Bypass Versus Roux-en-Y Gastric Bypass for Morbid Obesity: an Updated Meta-Analysis.Obes Surg. 2019 Sep;29(9):2721-2730. doi: 10.1007/s11695-019-04005-0. Obes Surg. 2019. PMID: 31172454
Cited by
-
Conversion of one-anastomosis gastric bypass to Roux-En-Y gastric bypass: mid-term results from the United Arab Emirates.Surg Endosc. 2025 Jan;39(1):417-424. doi: 10.1007/s00464-024-11271-2. Epub 2024 Oct 2. Surg Endosc. 2025. PMID: 39358568
References
-
- Voon K, Huang CK, Patel A, Wong LF, Lu YC, Hsin MC. Conversion of one-anastomosis gastric bypass (OAGB) to roux-en-Y gastric bypass (RYGB) is effective in dealing with late complications of OAGB: experience from a tertiary bariatric Center and literature review. J Metab Bariatr Surg 2021;10:32–41. - PMC - PubMed
-
- Mora Oliver I, Cassinello Fernández N, Alfonso Ballester R, Cuenca Ramírez MD, Ortega SJ. Revisional bariatric surgery due to failure of the initial technique: 25 years of experience in a specialized unit of obesity surgery in Spain. Cir Esp (Engl Ed) 2019;97:568–74 English, Spanish. - PubMed
-
- Jedamzik J, Bichler C, Felsenreich DM, Gensthaler L, Eichelter J, Nixdorf L, et al. Conversion from one-anastomosis gastric bypass to roux-en-Y gastric bypass: when and why-a single-center experience of all consecutive OAGB procedures. Surg Obes Relat Dis 2022;18:225–32. - PubMed
-
- Musella M, Susa A, Manno E, De Luca M, Greco F, Raffaelli M, et al. Complications following the mini/one anastomosis gastric bypass (MGB/OAGB): a multi-institutional survey on 2678 patients with a mid-term (5 years) follow-up. Obes Surg 2017;27:2956–67. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Research Materials

