Isoniazid and Rifampicin Resistance-Conferring Mutations in Mycobacterium tuberculosis Isolates from South Africa
- PMID: 37623975
- PMCID: PMC10458554
- DOI: 10.3390/pathogens12081015
Isoniazid and Rifampicin Resistance-Conferring Mutations in Mycobacterium tuberculosis Isolates from South Africa
Abstract
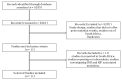
Tuberculosis (TB), caused by Mycobacterium tuberculosis (M. tb), remains a significant global health issue, with high morbidity and mortality rates. The emergence of drug-resistant strains, particularly multidrug-resistant TB (MDR-TB), poses difficult challenges to TB control efforts. This comprehensive review and meta-analysis investigated the prevalence of and molecular insights into isoniazid (INH) and rifampicin (RIF) resistance-conferring mutations in M. tb isolates from South Africa. Through systematic search and analysis of 11 relevant studies, we determined the prevalence of gene mutations associated with RIF and INH resistance, such as rpoB, katG, and inhA. The findings demonstrated a high prevalence of specific mutations, including S450L in rpoB, and S315T, which are linked to resistance against RIF and INH, respectively. These results contribute to the understanding of drug resistance mechanisms and provide valuable insights for the development of targeted interventions against drug-resistant TB.
Keywords: INH; RIF; drug resistance mechanisms; resistance-conferring mutations; tuberculosis.
Conflict of interest statement
The authors declare no conflict of interest.
Figures
References
-
- World Health Organization (WHO) Global Tuberculosis Report 2020. WHO; Geneva, Switzerland: 2020. [(accessed on 16 April 2021)]. Available online: https://www.who.int/publications/i/item/9789240013131.
-
- World Health Organization (WHO) Global Tuberculosis Report 2019. WHO; Geneva, Switzerland: 2019. [(accessed on 16 April 2021)]. Available online: https://www.who.int/publications/i/item/9789241565714.
-
- Cox H., Goig G.A., Salaam-Dreyer Z., Dippenaar A., Reuter A., Mohr-Holland E., Daniels J., Cudahy P.G., Nicol M.P., Borrell S., et al. Whole-genome sequencing has the potential to improve treatment for rifampicin-resistant tuberculosis in high-burden settings: A retrospective cohort study. J. Clin. Microbiol. 2022;60:e0236221. doi: 10.1128/jcm.02362-21. - DOI - PMC - PubMed
-
- Oostvogels S., Ley S.D., Heupink T.H., Dippenaar A., Streicher E.M., De Vos E., Meehan C.J., Dheda K., Warren R., Van Rie A. Transmission, distribution and drug resistance-conferring mutations of extensively drug-resistant tuberculosis in the Western Cape Province, South Africa. Microb. Genom. 2022;8:000815. doi: 10.1099/mgen.0.000815. - DOI - PMC - PubMed
Publication types
LinkOut - more resources
Full Text Sources