Technical Aspects and Clinical Limitations of Sperm DNA Fragmentation Testing in Male Infertility: A Global Survey, Current Guidelines, and Expert Recommendations
- PMID: 37635341
- PMCID: PMC10782128
- DOI: 10.5534/wjmh.230076
Technical Aspects and Clinical Limitations of Sperm DNA Fragmentation Testing in Male Infertility: A Global Survey, Current Guidelines, and Expert Recommendations
Abstract
Purpose: Sperm DNA fragmentation (SDF) is a functional sperm abnormality that can impact reproductive potential, for which four assays have been described in the recently published sixth edition of the WHO laboratory manual for the examination and processing of human semen. The purpose of this study was to examine the global practices related to the use of SDF assays and investigate the barriers and limitations that clinicians face in incorporating these tests into their practice.
Materials and methods: Clinicians managing male infertility were invited to complete an online survey on practices related to SDF diagnostic and treatment approaches. Their responses related to the technical aspects of SDF testing, current professional society guidelines, and the literature were used to generate expert recommendations via the Delphi method. Finally, challenges related to SDF that the clinicians encounter in their daily practice were captured.
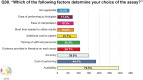
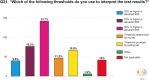
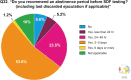
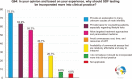
Results: The survey was completed by 436 reproductive clinicians. Overall, terminal deoxynucleotidyl transferase deoxyuridine triphosphate Nick-End Labeling (TUNEL) is the most commonly used assay chosen by 28.6%, followed by the sperm chromatin structure assay (24.1%), and the sperm chromatin dispersion (19.1%). The choice of the assay was largely influenced by availability (70% of respondents). A threshold of 30% was the most selected cut-off value for elevated SDF by 33.7% of clinicians. Of respondents, 53.6% recommend SDF testing after 3 to 5 days of abstinence. Although 75.3% believe SDF testing can provide an explanation for many unknown causes of infertility, the main limiting factors selected by respondents are a lack of professional society guideline recommendations (62.7%) and an absence of globally accepted references for SDF interpretation (50.3%).
Conclusions: This study represents the largest global survey on the technical aspects of SDF testing as well as the barriers encountered by clinicians. Unified global recommendations regarding clinician implementation and standard laboratory interpretation of SDF testing are crucial.
Keywords: DNA fragmentation; Delphi method; Diagnostic test; Infertility, male; Survey.
Copyright © 2024 Korean Society for Sexual Medicine and Andrology.
Conflict of interest statement
The authors have nothing to disclose.
Figures





Similar articles
-
Controversy and Consensus on Indications for Sperm DNA Fragmentation Testing in Male Infertility: A Global Survey, Current Guidelines, and Expert Recommendations.World J Mens Health. 2023 Jul;41(3):575-602. doi: 10.5534/wjmh.220282. Epub 2023 Apr 10. World J Mens Health. 2023. PMID: 37118960 Free PMC article.
-
Controversy and Consensus on the Management of Elevated Sperm DNA Fragmentation in Male Infertility: A Global Survey, Current Guidelines, and Expert Recommendations.World J Mens Health. 2023 Oct;41(4):809-847. doi: 10.5534/wjmh.230008. Epub 2023 Apr 20. World J Mens Health. 2023. PMID: 37118965 Free PMC article.
-
Sperm DNA fragmentation testing: a cross sectional survey on current practices of fertility specialists.Transl Androl Urol. 2017 Sep;6(Suppl 4):S710-S719. doi: 10.21037/tau.2017.06.21. Transl Androl Urol. 2017. PMID: 29082205 Free PMC article.
-
Sperm DNA damage and its impact on male reproductive health: a critical review for clinicians, reproductive professionals and researchers.Expert Rev Mol Diagn. 2019 Jun;19(6):443-457. doi: 10.1080/14737159.2019.1614916. Epub 2019 May 13. Expert Rev Mol Diagn. 2019. PMID: 31056976 Review.
-
Best laboratory practices and therapeutic interventions to reduce sperm DNA damage.Andrologia. 2021 Mar;53(2):e13736. doi: 10.1111/and.13736. Epub 2020 Jul 14. Andrologia. 2021. PMID: 32662555 Review.
Cited by
-
Revolutionizing Andrology: The Advent of the Global Andrology Forum, a Groundbreaking Initiative.World J Mens Health. 2025 Jan;43(1):1-7. doi: 10.5534/wjmh.240108. Epub 2024 Oct 15. World J Mens Health. 2025. PMID: 39434393 Free PMC article. No abstract available.
-
Reducing Quotation Errors in Scientific Manuscripts: A Novel Approach from the Global Andrology Forum.World J Mens Health. 2025 Jul;43(3):710-720. doi: 10.5534/wjmh.240255. Epub 2025 Jan 2. World J Mens Health. 2025. PMID: 39843175 Free PMC article.
-
Idiopathic male infertility - what are we missing?Arab J Urol. 2024 Jul 22;23(3):215-229. doi: 10.1080/20905998.2024.2381972. eCollection 2025. Arab J Urol. 2024. PMID: 40747475 Free PMC article.
-
The Andrological Landscape in the Twenty-First Century: Making Sense of the Advances in Male Infertility Management for the Busy Clinicians.Int J Environ Res Public Health. 2024 Sep 17;21(9):1222. doi: 10.3390/ijerph21091222. Int J Environ Res Public Health. 2024. PMID: 39338105 Free PMC article. Review.
-
Sperm DNA fragmentation in male infertility: From bench to bedside.Arab J Urol. 2023 Nov 23;21(4):199-203. doi: 10.1080/20905998.2023.2278200. eCollection 2023. Arab J Urol. 2023. PMID: 38178953 Free PMC article. Review.
References
-
- Meseguer M, Santiso R, Garrido N, Garcia-Herrero S, Remohi J, Fernandez JL. Effect of sperm DNA fragmentation on pregnancy outcome depends on oocyte quality. Fertil Steril. 2011;95:124–128. - PubMed
-
- Agarwal A, Hamada A, Esteves SC. Insight into oxidative stress in varicocele-associated male infertility: part 1. Nat Rev Urol. 2012;9:678–690. - PubMed

