Prescribing patterns of antihypertensive medications: A systematic review of literature between 2010 and 2020
- PMID: 37635839
- PMCID: PMC10448163
- DOI: 10.1016/j.rcsop.2023.100315
Prescribing patterns of antihypertensive medications: A systematic review of literature between 2010 and 2020
Abstract
Background: Hypertension has affected over 1.13 billion people worldwide in 2015 and it's one of the most preventable risk-factors for morbidity and mortality. Antihypertensives significantly reduce cardiovascular risks. Several studies on antihypertensives' prescribing patterns were conducted worldwide, and guidelines were developed on hypertension management. However, no systematic reviews were conducted globally to synthesize the evidence from these studies. This review aims to evaluate antihypertensives' prescription patterns, and adherence to international guidelines for hypertension management worldwide.
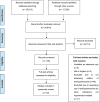
Methods: Full-text antihypertensives' prescribing patterns evaluation studies were included. Reviews, commentaries, guidelines, and editorials were excluded. Various databases were searched including PubMed, Embase, and others. Studies were limited to English only and to articles published from (01/01/2010) to (20/03/2020). Crowe Critical Appraisal Tool (CCAT) was used for quality assessment.
Results: The most commonly prescribed antihypertensives as monotherapy in adult patients with no comorbidities were ACEIs/ARBs (Angiotensin converting enzyme inhibitors/Angiotensin receptor blockers), followed by CCBs (Calcium channel blockers), and BBs (Beta Blockers). Most commonly prescribed dual combinations were thiazide diuretics+ACEIs/ARBs, BBs + CCBs and CCBs+ACEIs/ARBs. Among diabetic patients, the most common agents were ACEIs/ARBs. Among patients with heart diseases, CCBs were prescribed frequently. While patients with kidney diseases, CCBs and ARBs were most prescribed. Of the 40 studies included in the review, only four studies directly assessed the prescribing patterns of antihypertensives in adherence to clinical practice guidelines. And only two studies confirmed adherence to guidelines. Furthermore, the quality of the majority of studies was moderate (50%), while 25% of articles were reported as either high or low quality.
Conclusion: This review revealed that there are areas for improvement for prescribing practices of antihypertensives in concordance with the latest evidence and with clinical practice guidelines.
Keywords: Guidelines; Hypertension; Prescribing patterns; Review.
© 2023 The Authors.
Conflict of interest statement
Nothing to declare
References
-
- Hypertension Key Fact., Page Hypertension Key Fact. https://www.who.int/news-room/fact-sheets/detail/hypertension (Accessed 11 March 2020.
-
- Noncommunicable Diseases Country Profiles., Page Noncommunicable Diseases Country Profiles. https://www.who.int/nmh/publications/ncd-profiles-2018/en/ (Accessed 11 March 2020.
-
- EJ S.J. Maclaughlin., editor. Pharmacotherapy: A Pathophysiologic Approach. McGraw-Hill Education; New York: 2023. 11e NY.
-
- Ettehad D., Emdin C.A., Kiran A., et al. Blood pressure lowering for prevention of cardiovascular disease and death: a systematic review and meta-analysis. Lancet. 2016;387:957–967. - PubMed
Publication types
LinkOut - more resources
Full Text Sources