Posterior segment manifestations and imaging features post-COVID-19
- PMID: 37641707
- PMCID: PMC10460223
- DOI: 10.51329/mehdiophthal1427
Posterior segment manifestations and imaging features post-COVID-19
Abstract
Background: To report the posterior segment (uvea and retinal) manifestations and imaging characteristics of eyes of patients with and after coronavirus disease 2019 (COVID-19).
Methods: We searched the PubMed/MEDLINE database to identify relevant articles using the following search terms: COVID-19, SARS-CoV-2, retina, uvea, optic nerve, retinal findings, posterior segment manifestations, and endophthalmitis. Articles published from December 1, 2019, to May 30, 2021, and indexed in PubMed/ MEDLINE were screened.
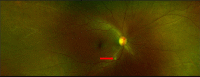
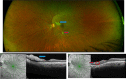
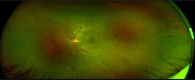
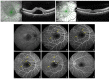
Results: For the purpose of this review, we included clinical features of 26 case reports and 8 case series. The posterior segment manifestations reported included cotton wool spots, retinal hemorrhages, central serous retinopathy, papillophlebitis, optic neuritis, panuveitis, multifocal retinitis, necrotizing retinitis, central retinal artery/vein occlusion, and Purtschner like retinopathy. In this review, we have also included optical coherence tomography angiography (OCTA) features that have been described in COVID-19 patients with pneumonia.
Conclusions: COVID-19 patients can experience uveo-retinal manifestations even after recovery. These patients, even if asymptomatic for eye symptoms, should undergo an eye evaluation to rule out posterior segment involvement. OCTA performed in these patients revealed microvascular changes in the superficial and deep retinal plexuses. Some of these patients may require anticoagulant or antiplatelet therapy.
Keywords: COVID-19; OCTA; SARS-CoV-2; ocular manifestations; optical coherence tomography angiography; posterior segment; retina; uvea.
© Author(s).
Conflict of interest statement
None
Figures
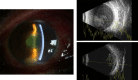
References
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous
