Assessing the reliability of CBCT-based AI-generated STL files in diagnosing osseous changes of the mandibular condyle: a comparative study with ground truth diagnosis
- PMID: 37641960
- PMCID: PMC10552125
- DOI: 10.1259/dmfr.20230141
Assessing the reliability of CBCT-based AI-generated STL files in diagnosing osseous changes of the mandibular condyle: a comparative study with ground truth diagnosis
Abstract
Objectives: This study aims to evaluate the reliability of AI-generated STL files in diagnosing osseous changes of the mandibular condyle and compare them to a ground truth (GT) diagnosis made by six radiologists.
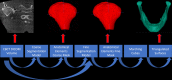
Methods: A total of 432 retrospective CBCT images from four universities were evaluated by six dentomaxillofacial radiologists who identified osseous changes such as flattening, erosion, osteophyte formation, bifid condyle formation, and osteosclerosis. All images were evaluated by each radiologist blindly and recorded on a spreadsheet. All evaluations were compared and for the disagreements, a consensus meeting was held online to create a uniform GT diagnosis spreadsheet. A web-based dental AI software was used to generate STL files of the CBCT images, which were then evaluated by two dentomaxillofacial radiologists. The new observer, GT, was compared to this new STL file evaluation, and the interclass correlation (ICC) value was calculated for each pathology.
Results: Out of the 864 condyles assessed, the ground truth diagnosis identified 372 cases of flattening, 185 cases of erosion, 70 cases of osteophyte formation, 117 cases of osteosclerosis, and 15 cases of bifid condyle formation. The ICC values for flattening, erosion, osteophyte formation, osteosclerosis, and bifid condyle formation were 1.000, 0.782, 1.000, 0.000, and 1.000, respectively, when comparing diagnoses made using STL files with the ground truth.
Conclusions: AI-generated STL files are reliable in diagnosing bifid condyle formation, osteophyte formation, and flattening of the condyle. However, the diagnosis of osteosclerosis using AI-generated STL files is not reliable, and the accuracy of diagnosis is affected by the erosion grade.
Keywords: artificial intelligence; cone-beam computed tomography; mandibular condyle; stereolithography; temporomandibular joint.
Conflict of interest statement
Conflict of interest statementAll authors declare that they have no conflict of interest.
Figures
Similar articles
-
Diagnostic performance of magnetic resonance imaging for detecting osseous abnormalities of the temporomandibular joint and its correlation with cone beam computed tomography.Dentomaxillofac Radiol. 2010 Jul;39(5):270-6. doi: 10.1259/dmfr/25151578. Dentomaxillofac Radiol. 2010. PMID: 20587650 Free PMC article.
-
Evaluation of the severity of temporomandibular joint osteoarthritic changes related to age using cone beam computed tomography.Dentomaxillofac Radiol. 2009 Mar;38(3):141-7. doi: 10.1259/dmfr/59263880. Dentomaxillofac Radiol. 2009. PMID: 19225084
-
The effect of myotonic dystrophy type 1 on temporomandibular joint and dentofacial morphology: A CBCT analysis.J Oral Rehabil. 2023 Oct;50(10):958-964. doi: 10.1111/joor.13533. Epub 2023 Jun 16. J Oral Rehabil. 2023. PMID: 37294889
-
Osseous abnormalities of the mandibular condyle: diagnostic reliability of cone beam computed tomography compared with helical computed tomography based on an autopsy material.Dentomaxillofac Radiol. 2006 May;35(3):152-7. doi: 10.1259/dmfr/15831361. Dentomaxillofac Radiol. 2006. PMID: 16618847
-
The diagnostic accuracy of cone-beam computed tomography for assessing in vitro osseous alterations of the mandibular condyle: a systematic review and meta-analysis.Oral Radiol. 2025 May 2. doi: 10.1007/s11282-025-00821-6. Online ahead of print. Oral Radiol. 2025. PMID: 40314859 Review.
Cited by
-
Concerns regarding deployment of AI-based applications in dentistry - a review.BDJ Open. 2025 Mar 25;11(1):27. doi: 10.1038/s41405-025-00319-7. BDJ Open. 2025. PMID: 40133287 Free PMC article. Review.
-
Automatic segmentation and visualization of cortical and marrow bone in mandibular condyle on CBCT: a preliminary exploration of clinical application.Oral Radiol. 2025 Jan;41(1):88-101. doi: 10.1007/s11282-024-00780-4. Epub 2024 Nov 9. Oral Radiol. 2025. PMID: 39520662
-
A Deep Learning Approach for Mandibular Condyle Segmentation on Ultrasonography.J Imaging Inform Med. 2025 May 6. doi: 10.1007/s10278-025-01527-1. Online ahead of print. J Imaging Inform Med. 2025. PMID: 40329156
References
-
- Schiffman E, Ohrbach R, Truelove E, Look J, Anderson G, Goulet J-P, et al. . Diagnostic criteria for Temporomandibular disorders (DC/TMD) for clinical and research applications: recommendations of the International RDC/TMD consortium network* and orofacial pain special interest group†. J Oral Facial Pain Headache 2014; 28: 6–27. doi: 10.11607/jop.1151 - DOI - PMC - PubMed
-
- Rozylo-Kalinowska I, Orhan K. Imaging of the Temporomandibular Joint. In: Imaging of the Temporomandibular Joint. Cham: Springer Nature; 2019. doi: 10.1007/978-3-319-99468-0 - DOI
MeSH terms
LinkOut - more resources
Full Text Sources
Miscellaneous