Value of Breast MRI and Nomogram After Negative Axillary Ultrasound for Predicting Axillary Lymph Node Metastasis in Patients With Clinically T1-2 N0 Breast Cancer
- PMID: 37644678
- PMCID: PMC10462481
- DOI: 10.3346/jkms.2023.38.e251
Value of Breast MRI and Nomogram After Negative Axillary Ultrasound for Predicting Axillary Lymph Node Metastasis in Patients With Clinically T1-2 N0 Breast Cancer
Abstract
Background: There are increasing concerns about that sentinel lymph node biopsy (SLNB) could be omitted in patients with clinically T1-2 N0 breast cancers who has negative axillary ultrasound (AUS). This study aims to assess the false negative result (FNR) of AUS, the rate of high nodal burden (HNB) in clinically T1-2 N0 breast cancer patients, and the diagnostic performance of breast magnetic resonance imaging (MRI) and nomogram.
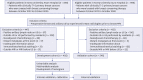
Methods: We identified 948 consecutive patients with clinically T1-2 N0 cancers who had negative AUS, subsequent MRI, and breast conserving therapy between 2013 and 2020 from two tertiary medical centers. Patients from two centers were assigned to development and validation sets, respectively. Among 948 patients, 402 (mean age ± standard deviation, 57.61 ± 11.58) were within development cohort and 546 (54.43 ± 10.02) within validation cohort. Using logistic regression analyses, clinical-imaging factors associated with lymph node (LN) metastasis were analyzed in the development set from which nomogram was created. The performance of MRI and nomogram was assessed. HNB was defined as ≥ 3 positive LNs.
Results: The FNR of AUS was 20.1% (81 of 402) and 19.2% (105 of 546) and the rates of HNB were 1.2% (5/402) and 2.2% (12/546), respectively. Clinical and imaging features associated with LN metastasis were progesterone receptor positivity, outer tumor location on mammography, breast imaging reporting and data system category 5 assessment of cancer on ultrasound, and positive axilla on MRI. In validation cohorts, the positive predictive value (PPV) and negative predictive value (NPV) of MRI and clinical-imaging nomogram was 58.5% and 86.5%, and 56.0% and 82.0%, respectively.
Conclusion: The FNR of AUS was approximately 20% but the rate of HNB was low. The diagnostic performance of MRI was not satisfactory with low PPV but MRI had merit in reaffirming negative AUS with high NPV. Patients who had low probability scores from our clinical-imaging nomogram might be possible candidates for the omission of SLNB.
Keywords: Axilla; Breast Neoplasms; Lymphatic Metastasis; Nomogram; Ultrasonography.
© 2023 The Korean Academy of Medical Sciences.
Conflict of interest statement
The authors have no potential conflicts of interest to disclose.
Figures



Similar articles
-
Breast cancer patients with a negative axillary ultrasound may have clinically significant nodal metastasis.Breast Cancer Res Treat. 2021 Jun;187(2):303-310. doi: 10.1007/s10549-021-06194-8. Epub 2021 Apr 10. Breast Cancer Res Treat. 2021. PMID: 33837870 Review.
-
A comparative analysis of axillary nodal burden in ultrasound/biopsy positive axilla vs ultrasound negative sentinel lymph node biopsy positive axilla.Breast Dis. 2019;38(3-4):93-96. doi: 10.3233/BD-160230. Breast Dis. 2019. PMID: 30909179
-
Axillary ultrasound after neoadjuvant therapy reduces the false-negative rate of sentinel lymph node biopsy in patients with cytologically node-positive breast cancer.Breast Cancer Res Treat. 2023 Feb;197(3):515-523. doi: 10.1007/s10549-022-06817-8. Epub 2022 Dec 13. Breast Cancer Res Treat. 2023. PMID: 36513955
-
Axillary Ultrasound Accurately Excludes Clinically Significant Lymph Node Disease in Patients With Early Stage Breast Cancer.Ann Surg. 2016 Dec;264(6):1098-1102. doi: 10.1097/SLA.0000000000001549. Ann Surg. 2016. PMID: 26779976 Free PMC article.
-
Cost-effectiveness analyses demonstrate that observation is superior to sentinel lymph node biopsy for postmenopausal women with HR + breast cancer and negative axillary ultrasound.Breast Cancer Res Treat. 2020 Sep;183(2):251-262. doi: 10.1007/s10549-020-05768-2. Epub 2020 Jul 10. Breast Cancer Res Treat. 2020. PMID: 32651755 Free PMC article. Review.
Cited by
-
Prediction of axillary nodal burden using preoperative magnetic resonance imaging scoring in patients with clinically node-negative breast cancer: a retrospective cohort study.Gland Surg. 2024 Dec 31;13(12):2288-2299. doi: 10.21037/gs-24-379. Epub 2024 Dec 27. Gland Surg. 2024. PMID: 39822365 Free PMC article.
References
-
- Caudle AS, Cupp JA, Kuerer HM. Management of axillary disease. Surg Oncol Clin N Am. 2014;23(3):473–486. - PubMed
-
- Burak WE, Jr, Hollenbeck ST, Zervos EE, Hock KL, Kemp LC, Young DC. Sentinel lymph node biopsy results in less postoperative morbidity compared with axillary lymph node dissection for breast cancer. Am J Surg. 2002;183(1):23–27. - PubMed
-
- Lyman GH, Giuliano AE, Somerfield MR, Benson AB, 3rd, Bodurka DC, Burstein HJ, et al. American society of clinical oncology guideline recommendations for sentinel lymph node biopsy in early-stage breast cancer. J Clin Oncol. 2005;23(30):7703–7720. - PubMed
-
- Giuliano AE, Ballman KV, McCall L, Beitsch PD, Brennan MB, Kelemen PR, et al. Effect of axillary dissection vs no axillary dissection on 10-year overall survival among women with invasive breast cancer and sentinel node metastasis: the ACOSOG Z0011 (Alliance) randomized clinical trial. JAMA. 2017;318(10):918–926. - PMC - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials

