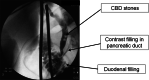
Pancreatic duct filling during cholecystectomy intraoperative cholangiogram and incidence of postoperative pancreatitis
- PMID: 37649861
- PMCID: PMC10463016
- DOI: 10.1002/jgh3.12954
Pancreatic duct filling during cholecystectomy intraoperative cholangiogram and incidence of postoperative pancreatitis
Abstract
Background and aim: Laparoscopic cholecystectomy (LC) with intraoperative cholangiography (IOC) is a commonly performed surgical procedure in most hospitals. Anecdotal evidence suggests that when the pancreatic duct (PD) inadvertently fills during IOC, there may be an increased risk of postoperative pancreatitis (POP). However, there is a paucity of information in the literature about both the incidence of pancreatitis post LC and the incidence of PD filling on IOC and any potential relationship between the two.
Methods: A retrospective review was performed of all LC performed in our institution over a 10-year period. IOC images were reviewed and clinical data collated.
Results: Of the 1243 procedures identified, 952 had IOC images available for review and were included in the study. The incidence of POP was 0.7%. The incidence of PD filling was 13.4%. Patient's age, sex, urgency of surgery, preoperative liver function tests (LFTs), history of pancreatitis, contrast leakage, and preoperative endoscopic retrograde cholangiopancreatography (ERCP) were not statistically related to the incidence of POP. Of those with PD filling, 2% had POP versus 0.5% who had no PD filling. This trended toward significance on univariate analysis (P = 0.05). However, on logistic regression, POP was the only significant independent risk factor (P = 0.02).
Conclusion: The incidence of pancreatitis post LC and IOC is low. PD filling is associated with increased incidence of pancreatitis in this scenario and it is crucial for clinicians to be aware of this potential risk. This retrospective study was based on the review of saved images, and therefore PD filling might have been underestimated. Prospective studies would be useful to ascertain any definitive clinical association.
Keywords: cholecystectomy; contrast reflux; intraoperative cholangiogram; pancreatitis.
© 2023 The Authors. JGH Open published by Journal of Gastroenterology and Hepatology Foundation and John Wiley & Sons Australia, Ltd.
Figures
Similar articles
-
Comparison of preoperative endoscopic retrograde cholangiopancreatography and laparoscopic cholecystectomy with operative management of gallstone pancreatitis.Am J Surg. 1997 Dec;174(6):719-22. doi: 10.1016/s0002-9610(97)00216-x. Am J Surg. 1997. PMID: 9409604
-
A practical cost-effective management strategy for gallstone pancreatitis.Am J Surg. 2013 Oct;206(4):472-7. doi: 10.1016/j.amjsurg.2012.12.009. Epub 2013 Apr 28. Am J Surg. 2013. PMID: 23631907
-
Incidence of residual choledocholithiasis detected by intraoperative cholangiography at the time of laparoscopic cholecystectomy in patients having undergone preoperative ERCP.Surg Endosc. 2008 Nov;22(11):2365-72. doi: 10.1007/s00464-008-9785-3. Epub 2008 Mar 6. Surg Endosc. 2008. PMID: 18322745
-
Management of suspected common bile duct stones in children: role of selective intraoperative cholangiogram and endoscopic retrograde cholangiopancreatography.J Pediatr Surg. 2004 Jun;39(6):808-12; discussion 808-12. doi: 10.1016/j.jpedsurg.2004.02.019. J Pediatr Surg. 2004. PMID: 15185201 Review.
-
Laparoscopic common bile duct exploration plus cholecystectomy versus endoscopic retrograde cholangiopancreatography plus laparoscopic cholecystectomy for cholecystocholedocholithiasis: a meta-analysis.Surg Endosc. 2019 Oct;33(10):3275-3286. doi: 10.1007/s00464-018-06613-w. Epub 2018 Dec 3. Surg Endosc. 2019. PMID: 30511313 Review.
References
-
- Caratozzolo E, Massani M, Recordare A et al. Usefulness of both operative cholangiography and conversion to decrease major bile duct injuries during laparoscopic cholecystectomy. J. Hepatobiliary Pancreat. Surg. 2004; 11: 171–175. - PubMed
-
- Ueno K, Ajiki T, Murakami S et al. Clinical significance of bile reflux into the pancreatic duct without pancreaticobiliary maljunction assessed by intraoperative cholangiography. Asian J. Endosc. Surg. 2015; 8: 296–302. - PubMed
-
- Fujisaki S, Tomita R, Koshinaga T, Fukuzawa M. Analysis of pancreaticobiliary ductal union based on intraoperative cholangiography in patients undergoing laparoscopic cholecystectomy. Scand. J. Gastroenterol. 2002; 37: 956–959. - PubMed
LinkOut - more resources
Full Text Sources