Continued Stabilization of a Cementless 3D-Printed Total Knee Arthroplasty: Five-Year Results of a Randomized Controlled Trial Using Radiostereometric Analysis
- PMID: 37651549
- PMCID: PMC10609712
- DOI: 10.2106/JBJS.23.00221
Continued Stabilization of a Cementless 3D-Printed Total Knee Arthroplasty: Five-Year Results of a Randomized Controlled Trial Using Radiostereometric Analysis
Abstract
Background: Three-dimensional (3D) printing of highly porous orthopaedic implants aims to promote better osseointegration, thus preventing aseptic loosening. However, short-term radiostereometric analysis (RSA) after total knee arthroplasty (TKA) has shown higher initial migration of cementless 3D-printed tibial components compared with their cemented counterparts. Therefore, critical evaluation of longer-term tibial component migration is needed. We investigated migration of a cementless 3D-printed and a cemented tibial component with otherwise similar TKA design during 5 years of follow-up, particularly the progression in migration beyond 2 years postoperatively.
Methods: Seventy-two patients were randomized to a cementless 3D-printed Triathlon Tritanium (Stryker) cruciate-retaining (CR) TKA or a cemented Triathlon CR (Stryker) TKA implant. Implant migration was evaluated with RSA at baseline and postoperatively at 3 months and at 1, 2, and 5 years. The maximum total point motion (MTPM) of the tibial component was compared between the groups at 5 years, and progression in migration was assessed between 2 and 5 years. Individual implants were classified as continuously migrating if the MTPM was ≥0.1 mm/year beyond 2 years postoperatively. Clinical scores were evaluated, and a linear mixed-effects model was used to analyze repeated measurements.
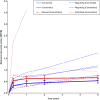
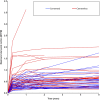
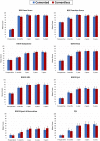
Results: At 5 years, the mean MTPM was 0.66 mm (95% confidence interval [CI], 0.56 to 0.78 mm) for the cementless group and 0.53 mm (95% CI, 0.43 to 0.64 mm) for the cemented group (p = 0.09). Between 2 and 5 years, there was no progression in mean MTPM for the cementless group (0.02 mm; 95% CI, -0.06 to 0.10 mm) versus 0.07 mm (95% CI, 0.00 to 0.14) for the cemented group. One implant was continuously migrating in the cementless group, and 4 were continuously migrating in the cemented group. The clinical scores were comparable between the groups across the entire time of follow-up.
Conclusions: No significant difference in mean migration was found at 5 years between the cementless and cemented TKA implants. Progression of tibial component migration was present beyond 2 years for the cemented implant, whereas the cementless implant remained stable after initial early migration.
Level of evidence: Therapeutic Level I . See Instructions for Authors for a complete description of levels of evidence.
Copyright © 2023 The Authors. Published by The Journal of Bone and Joint Surgery, Incorporated. All rights reserved.
Conflict of interest statement
Disclosure: The Disclosure of Potential Conflicts of Interest forms are provided with the online version of the article ( http://links.lww.com/JBJS/H671 ).
Figures

References
-
- American Joint Replacement Registry (AJRR). 2022. Annual Report 2022. Accessed 2023 Jul 21. https://www.aaos.org/registries/publications/ajrr-annual-report/.
-
- The Swedish Knee Arthroplasty Register. Annual Report 2020. 2020. Accessed 2023 Jul 21. https://www.myknee.se/en/.
-
- Dalury DF. Cementless total knee arthroplasty: current concepts review. Bone Joint J. 2016. Jul;98-B(7):867-73. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials

